- Acne inversa sufferers are faced with recurrent and often debilitating outbreaks that dramatically reduce their quality of life.
- Knowing which stage your acne inversa is in could help inform treatment options.
- No one knows for certain what causes acne inversa, but medical professionals believe that it could be linked to excessive sweating or changes in hormones.
- Although there is no cure for acne inversa, there are a variety of surgical and non-surgical treatments that can help manage the symptoms.
If you have acne inversa, or think that you might, read on to learn more about how this disease operates and what you can do to ensure a brighter future.
Understanding Acne Inversa
Acne inversa is a painful inflammatory skin condition that causes pus-filled pockets to appear under the skin. These pockets can be likened to boils or abscesses, although they are typically free of bacteria.
Acne inversa is perhaps a misnomer for this chronic and often debilitating skin condition. It is more commonly called hidradenitis suppurativa, and sometimes referred to as Verneuil’s Disease or Velpeau’s Disease.
While the direct causes of acne inversa are up for debate, medical professionals generally conclude that the condition occurs when hair follicles or glands — typically sweat glands — become blocked. This leads to inflammation, which in turn causes the pus-filled growths to appear, most commonly in areas of the body where sweat tends to accumulate.
These areas include the armpits, under the breasts, the groin, the buttocks, and the inner thighs, leading some researchers to believe that excessive sweating could be a risk factor for developing the disease.
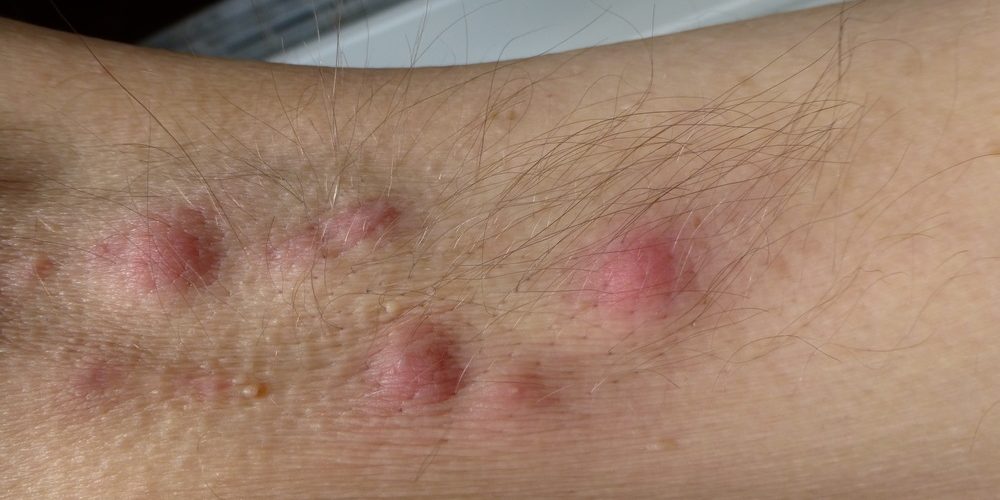
The Lifecycle of an Outbreak
Acne inversa comes in waves of outbreaks. These outbreaks vary dramatically in their severity and in the amount of time between episodes, but they usually follow the same general pattern.
At the onset of the outbreak, there is typically a single boil or abscess under the skin, presumably due to a clogged gland or follicle. The pus-filled growth hardens over time and becomes increasingly painful and inflamed.
Eventually it breaks open from the surface and leaks pus. Sometimes, these “open wounds” are resistant to healing, often resulting in scarring.
As outbreaks continue, sufferers from the condition may notice tunneling/grooves under the skin that connects the abscesses. This tunneling is called a sinus tract, and is a defining feature of more advanced stages of the condition.
Hurley’s Staging System
As with most skin conditions, the severity of acne inversa is categorized according to Hurley’s Staging System. Knowing which stage your acne inversa is in could help inform treatment options.
- Stage One – This stage typically involves very few abscesses or boils. The growths are widely spaced, don’t touch, and there is no sinus tract under the skin. At this stage, acne inversa is difficult to diagnose and is often mistaken for a bad case of acne.
- Stage Two – Abscesses continue to come back (recurring outbreaks); sinus tracts begin to develop; growths continue to be widely spaced and sparse.
- Stage Three – Abscesses are so large and plentiful that they begin to connect and nearly touch. Sinus tract formation is advanced and pervasive. Inflammation is serious and painful, significantly impacting quality of life. There may be some infection.
Typically, those with acne inversa in the first stage only resort to noninvasive skin treatments. However, by the third stage, surgical intervention is often necessary.
Where Acne Inversa Comes From
We’ve already established that acne inversa is believed to begin with a clogged duct or hair follicle. But how do these ducts or follicles get clogged in the first place? The truth is that no one really knows for certain.
Medical professionals theorize that excessive sweating or changes in hormones could be likely culprits, especially given the most common locations on the body for outbreaks and the fact that there are no reported cases prior to puberty.
Other potential causes include the dysfunctional production of androgen in the body and genetic disorders that affect cellular structures.
The disease has no clear risk factors when it comes to race. However, women tend to be somewhat more vulnerable to it, as well as adults in their twenties. Other risk factors include obesity, smoking, and having a family member with the disease.
Acne inversa has also been linked to other conditions, such as inflammatory bowel syndrome (IBS), Crohn’s Disease, and even arthritis.
Outbreak Triggers
If you’ve already been diagnosed with acne inversa, you may notice that your outbreak periods are linked to certain triggers and external factors.
- Stress – Anxiety and lengthy periods of stress can cause flare ups.
- Hormones – Outbreaks are sometimes known to flare with the menstrual cycle. Oral contraceptives are also linked to outbreaks.
- Heat and humidity – Dry and arid climates are ideal for managing outbreaks.
- Clothing – Tight clothing or clothing that causes a lot of friction can make outbreaks worse.
- Deodorant – Certain types of deodorant may aggravate the condition.
- Shaving the affected area – Friction and irritation from shaving can cause an outbreak.
- Obesity – Weight gain is common among those with the disease due to discomfort with exercise. However, obesity can also make the condition worse and trigger more frequent and more severe outbreaks.
Avoiding these triggers may help reduce the frequency and severity of outbreaks, but it will not cure you of the disease. Paying attention to trigger and avoiding them is key for managing the condition and improving your quality of life.
What to Expect from Acne Inversa
Aside from the typical symptoms and the progression of the illness already described, you can expect a variety of side effects and complications from this skin disease. Many of the following “side effects” are almost a guarantee if you have acne inversa. Others come about only in the most extreme cases.
It’s important to note that it’s difficult to pin down direct side effects of the disease. Many of these side effects are actually complications from chronic infection. What’s more, some correlations between acne inversa and other conditions are left off of this list.
For example, many people with acne inversa suffer from obesity, leading to a correlation between acne inversa and heart disease. We’ve reduced our list to the most direct (except where infections are involved) and the most common.
- Scarring – Open sores caused by abscesses breaking open can lead to severe and often raised scars. Severe scarring can also lead to discoloration of the skin (alopecia).
- Infections – Open sores can also lead to infection, particularly if they refuse to heal or there is a large number of them. If persistent or untreated, these may lead to sepsis.
- Cellulitis – This bacterial skin infection is the most commonly occurring in those with acne inversa.
- Joint pain – This is often caused by inflammation and may be persistent.
- Contracture – This is when muscles tighten or shorten, causing severely reduced mobility.
- Anemia – This is characterized by a low concentration of red blood cells in the blood. This can result from long-term and chronic infections.
- Hypoproteinemia – This refers to low levels of protein in the body and can result from severe and chronic infections.
- Obesity – Many people who suffer from acne inversa find significant movement painful, let along aerobic exercise. This puts them at a greater risk of obesity.
- Depression – This varies depending on the disease severity. However, with reduced mobility, pain, and the embarrassment of unsightly sores comes the inclination to seclude oneself, lethargy, and depression.
- Cancer – Don’t be alarmed. There is no firm proof that severe hidradenitis suppurativa and skin cancer are linked. However, some researchers have concluded from various case reports that there may be a link.
Acne inversa is not considered a life-threatening condition, although complications can lead to death in extreme circumstances. For example, low protein levels in the body can lead to renal failure (kidney failure). What’s more, extreme infections can be difficult to fight off for people with weakened immune systems.
Non-Surgical Treatments for Acne Inversa
Although there is no cure for acne inversa, there are a variety of treatments and techniques for managing outbreaks and mitigating discomfort. These treatments vary from simple topical ointments to invasive surgery. Here we’ll explore those nonsurgical treatments best suited to someone in Hurley Stage I or II of the condition.
- Loose clothing — Avoid friction. Look for fabrics that breathe. You may also consider leaving the area exposed if possible.
- General hygiene — Clean and dry the area multiple times a day. Pat the affected area; do not use friction.
- Weight management — Eating healthy and light activity will help prevent obesity. Weight loss may also be in order.
- Sweat reduction — Keep the area cool. Avoid excessive heat and humidity.
- Dairy reduction — Dairy can affect hormones, which in turn affect outbreak frequency and severity. Reduce or eliminate dairy intake.
- Antiseptic cleansers — Antiseptics reduce the risk of infection. Use them sparingly and heavily diluted.
- Hydrogen Peroxide — This is also effective in preventing infection in minor injuries.
- Hip baths – Warm baths can help treat the pain and inflammation associated with outbreaks. Hip baths, also known as Sitz baths, involve sitting in warm water up to the waist. These are effective in soothing outbreaks below the waist.
- Vinegar baths — Some people have suggested adding distilled white vinegar to a bath for added comfort and hygiene.
In short, these milder treatments involve keeping the affected location clean and dry. Baths should be used sparingly and the area should be thoroughly dried afterward.
If your acne inversa is unresponsive to these treatments, you may be prescribed a medication, especially if you’re determined to be in Hurley Stage II of the condition.
- Antibiotics — Simply put, if you have an infection, these will treat it. By reducing the symptoms associated with infection, they may provide some relief, but they are not effective against outbreaks themselves. Topical antibiotics are usually most effective.
- Corticosteroids — These can be topical or ingested. Corticosteroids mimic the body’s natural hormones, only in larger doses. They help the body manage inflammation, infection, protein balance, and more.
- Anti-inflammatories — Doctors may prescribe over-the-counter anti-inflammatory painkillers, such as ibuprofen, in significantly larger dosages.
- TNF Inhibitors — These anti-inflammatory drugs specifically target the tumor necrosis factor (TNF). TNF is a part of the inflammatory process that can lead to cell death (necrosis). It’s common among many autoimmune disorders and disorders centered around persistent inflammation, including acne inversa.
As with the other non-invasive treatments listed here, there is no medication that can cure the disease. Medications can be prescribed purely for pain and symptom management.
Surgical Treatments for Acne Inversa
If you’re at the third stage of the disease and other less invasive methods have proved fruitless, you may consider a variety of surgical options, beginning with simple laser hair removal and ending with radical excision of the entire affected area.
Going under the knife may feel like an extreme response to a skin condition. However, surgery for acne inversa has seen some significant success and could make for a dramatic improvement in quality of life.
- Laser hair removal
This destroys the hair follicles in the affected tissue. Given that clogged and inflamed follicles are suspected as triggers for the disease, this is seen as a method for not only clearing up existing breakouts, but also preventing future ones. It may need to be done several times.
- Local incision and drainage
This method is only helpful for short-term relief when an outbreak becomes particularly painful. The surgeon cuts open the lesion and drains it. This effectively speeds up the progression of the outbreak cycle (see above), reducing pain causes by pressure and inflammation.
- Deroofing of lesions
Instead of just training lesions, surgeons can surgically remove the tops of the lesions. This may cause scarring, but it also leads to healing, reduced inflammation, and reduced pain. Sometimes this is done as a preliminary measure for more involved surgeries.
- Removal of fistula and sinus tracts
Fistula tracts are similar to sinus tracts. In fact, the terms are often used interchangeably. However, fistula technically connect two organs or body cavities, or connect a cavity to the surface of the skin. A sinus tract may connect two spaces or begin in one space and reach a dead end inside the body.
Typically, when talking about acne inversa, the cavities that form between abscesses are referred to as sinus tract, but they could qualify as either. Surgery that seeks to remove these tracks will inject dye into the skin to reveal the subcutaneous tracts. The surgeon then removes all areas revealed in this way.
- Radical excision
This extreme measure involves cutting into the skin and removing the entire affected area. It is reserved only for more severe cases and recurring cases. The incision is deep and will go about 2 centimeters beyond the affected area in all directions.
This surgery removes all elements of the disease, including abscesses and sinus tracts. The surgeon then applies skin grafts to the surgical site.
It sounds intense, but radical excision is the only method that has actually been known to “cure” the disease. It is by no means a reliable cure, and those who get it performed may still have a recurrence long after. For that reason, it’s no true cure. However, many patients have reported a complete reversal, stating that they no longer suffered from the condition after the surgery was performed.
- Electrosurgery (STEEP)
This method attempts to excise the affected area using a series of surgical peels that gradually strip away layers of tissue. Like radical excision, it cuts into the healthy layers of tissue in order to ensure that the entire affected area has been removed.
However, it is more precise and is able to spare more healthy tissue than radical excision. It’s also associated with shorter recovery times.
- Carbon dioxide laser
This is not so much a method as a tool. The carbon dioxide laser can be used for radical incision or for minor incisions as described above. It is effective but not particularly successful when it comes to preserving as much healthy tissue as possible.
Acne inversa, though rare, is not as rare as people once thought. It used to be that only the most extreme cases were seen, as those afflicted with the condition often hid it from embarrassment and only sought medical help when it got unbearable.
These days, we know that there are more people out there who are suffering in silence. Don’t wait to seek medical attention. Your prognosis with any of the methods described in this article will be significantly better if you start fighting back now.