- Bell’s palsy is the number one cause of facial paralysis in the United States.
- The condition affects the nerve that controls movement of muscles in the face.
- Most people with Bell’s Palsy make a complete recovery.
- About 10% of patients only recover partially while 5% require surgical intervention.
Bell’s palsy is the most common cause of facial paralysis, affecting around 40,000 Americans every year. It usually has a quick onset – someone may go to sleep and then wake up not being able to move one side of the face.
As alarming as this seems, the condition usually resolves on its own. If it doesn’t, there are medical and surgical avenues available to sufferers who have symptoms that persist.
Underlying causes and symptoms
Many ancient physicians, including Greek and Persian doctors, provided early clinical descriptions of this condition.
In the 19th century, a Scottish surgeon named Sir Charles Bell described the anatomy of the facial nerves, outlining the difference between sensory nerves and motor nerves in the spinal cord.
Bell’s palsy results from a dysfunction of cranial nerve VII, the facial nerve that transmits signals between the brain and the muscles of the face.
These muscles control facial expressions – everything from smiling, scowling, raising eyebrows and wrinkling the forehead – essential components of unspoken human communication.
Gone viral
Most scientists believe that a virus causes Bell’s palsy, although the mechanism is not well understood. Bell’s palsy affects men and women of any age but most commonly those between the ages of 15 and 60 years. People who are pregnant or have diabetes appear to be more affected.
Some of the culprits linked to Bell’s palsy include the viruses that cause:
- Mononucleosis, or “mono” (Epstein-Barr)
- Flu (influenza B)
- Hand-foot-mouth disease (Coxsackie)
- Chickenpox and shingles (herpes zoster)
- Cold sores and genital herpes (herpes simplex)
- Respiratory illnesses (adenovirus)
- German measles (rubella)
- Mumps (mumps virus)
Hallmark signs
In Bell’s palsy, the facial nerve becomes swollen or inflamed, leading to sudden facial weakness or paralysis. This translates to the inability to move muscles – usually, just on one side of the face.
Since the facial nerve is complex, nerve damage can lead to a number of problems that vary from patient to patient. These symptoms typically occur suddenly and may include:
- The face feeling stiff or pulled to one side
- Mild weakness to total paralysis on one side of the face
- Muscle twitching and/or weakness
- Problems smiling or making facial expressions
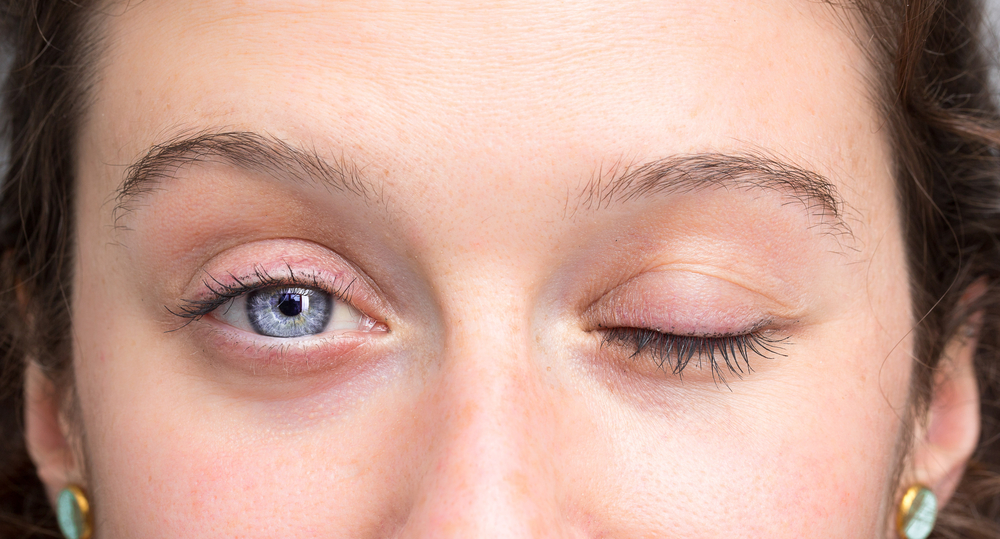
- Drooping or difficulty closing the eyelid
- Drooping of the corner of the mouth
- Difficulty eating and drinking
- Dryness of the eye or mouth
- Changes in the ability to taste
- Changes in the amount of tears and saliva produced
- Headaches, pain around the jaw or sensitivity to sound on the affected side.
Ruling out other causes
Bell’s palsy is not related to stroke – a condition where the blood supply to a part of the brain is interrupted, preventing brain cells from receiving enough oxygen and nutrients.
A stroke is a medical emergency. Within minutes, brain cells with no blood supply begin to die. Bell’s palsy, however, does not affect the brain. It only impacts the facial nerve. Someone with facial paralysis still needs to go to an emergency room or see a doctor immediately to rule out stroke or other underlying conditions, such as a tumor or Lyme disease.
After a diagnosis of Bell’s palsy is confirmed, it’s important to schedule a follow-up with an experienced facial paralysis expert. Dr. Babak Azizzadeh, who practices in Beverley Hills and is associated with the Facial Paralysis Institute, is a renowned specialist in facial paralysis treatment.
“The most important aspect of the evaluation is to perform an excellent neurologic and head and neck examination to make sure there aren’t any neurologic deficits,” Dr. Azizzadeh says. He may also order certain tests in some patients, including:
- Blood tests to rule out Lyme disease caused by a type of bacteria transmitted by ticks
- Magnetic resonance imaging (MRI) or computed tomography (CT) scan to rule out brain tumors or other neurological abnormalities
- Electrical testing like electromyography (EMG) to check the way muscles and nerve cells are conducting electrical signals
- Electroneurography (ENoG), a special test to specifically check the function of the facial nerve
Err on the side of caution
Although in most cases, these additional tests aren’t necessary, they may be needed if symptoms don’t subside over time.
Dr. Azizzadeh notes that “many people who get Bell’s palsy make a full recovery in the first 12 months.” A year may seem like a long time to some of his patients, but he advises against pursuing invasive treatments before a year. However, he does assess each patient on a case by case basis, and likes to monitor progress in order to make any necessary recommendations.
As soon as a diagnosis of Bell’s palsy is confirmed, Dr. Azizzadeh is likely to “prescribe a high dose of steroids as well as an anti-viral medication such as Valtrex. Time is of the essence.” He prefers starting medications quickly so the steroids can reduce the inflammation and the anti-viral medication can stop whatever virus may be causing it.
If necessary, long-term treatment options may be pursued following these immediate actions.
Overcoming unresolved symptoms
Unfortunately, not all Bell’s palsy patients make a full recovery in their first year. They may have residual symptoms, like an eyelid droop or a lopsided smile. Even subtle asymmetries in the face can be very noticeable, affecting social interactions and self-esteem.
Patients with Bell’s palsy usually fall into three groups:
- 85% have a complete recovery within days or months with no lingering issues.
- 10% undergo a partial recovery, with continued facial weakness or misdirected regrowth of nerve fibers called synkinesis (i.e. the damaged facial nerve grows back into the wrong areas of the face, which causes muscle misfiring or twitching).
- 5% have complete facial paralysis or almost no improvement of symptoms, and significant synkinesis.
Complications from Bell’s palsy may include irreversible damage to the facial nerve or mis-coordination of facial muscle movements as well as damage to the cornea (clear protective cover of the eye) if it affects the eyelid’s ability to close.
Surgical and non-invasive treatment options
For patients with residual symptoms, there are various non-invasive treatment options available. These include:
• Facial physical therapy to build up coordination and strength in the facial muscles.
• Treatment with Botox to stop unwanted muscle movements, especially in cases of synkinesis or rewiring of the facial nerve.
• Injectable fillers to improve facial asymmetry.
Board-certified plastic surgeon Dr. Steven Davis in Cherry Hill, New Jersey explains that if “Bell’s palsy is still present, we can use a neuromodulator, such as Botox, and inject the opposite side of the face where the Bell’s palsy occurs so it’s less obvious that a laziness or drooping of the face exists.”
There are also surgical options for the 5-15% of patients who need intervention.
Selective neurolysis involves mapping out facial nerves, releasing one of the frowning muscles and rerouting the facial nerve. A cross facial nerve graft involves taking a section of nerve from somewhere else in the body – usually the leg – and using it as a conduit or bridge from the normal facial nerve to the other side of the face that’s affected by Bell’s palsy.
It takes nerve to ask for help
There is ongoing research on new effective treatments for Bell’s palsy. If you have symptoms that persist, know that there is help available. Reaching out to find out what options are available is an important first step.
» For more information on cosmetic treatments for residual Bell’s palsy symptoms, meet our Medical Review Team.