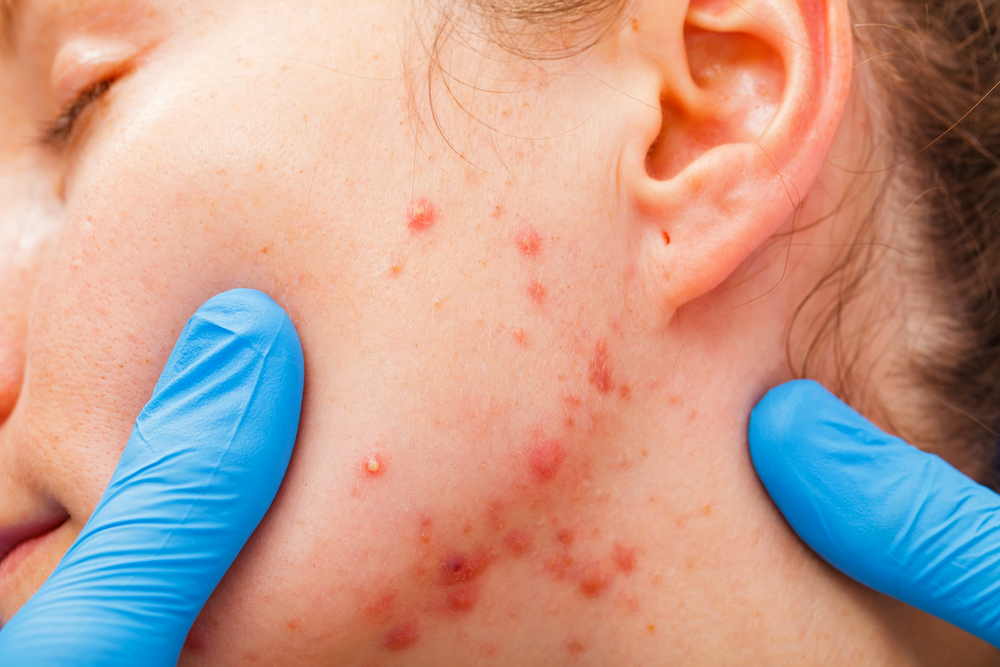
- Cystic acne is a severe form of acne that manifests as large, red, tender bumps deep within the skin.
- Cystic acne is painful and difficult to cure, causing blemishes that may linger for months.
- Effective treatments include oral isotretinoin, birth control pills, and topical retinoids.
What is cystic acne?
In general, acne occurs when skin’s pores become blocked with oil, dead skin cells or bacteria. Acne comes in a variety of forms, including whiteheads, blackheads, pimples, and nodules—large fluid-filled bumps deep within the skin.
Cystic acne occurs when bacteria gets deep down into the skin and becomes infected, forming a cyst (or large, red, tender bump) that doesn’t come to a head.
Unlike pimples, which usually disappear in a matter of days, cysts may linger for weeks or even months.
Cystic acne is usually found on the face, but it can also appear on the chest, neck, back, arms, and even on the shoulders and behind the ears. Cystic acne blemishes may itch and be quite painful—another defining symptom.
» Learn more about the causes and treatment options for back and chest acne
What causes cystic acne?
Most people who develop cystic acne do so in their teens or early 20s. However, it can strike at any age, and some people (especially women) find themselves developing this acne well into adulthood, even if they had clear skin as a teenager.
As with other forms of acne, many different factors interact to cause cystic acne, including hormones, genetics, and environment.
Hormones
Hormones are a known trigger of acne in general. Varying levels of estrogen, testosterone, and androgen can all play a role in the development of acne. As testosterone levels rise during puberty, sebaceous glands produce more sebum—an oily waxy substance—that can contribute to blocked pores and result in acne.
Women frequently find that cysts flare up during their monthly menstrual cycle alongside other types of acne.
“Adult female acne tends to be more cystic in nature, suggesting that androgen hormones can influence this clinical picture,” says Dr. Adam Friedman, Associate Professor of Dermatology at the George Washington University School of Medicine & Health Sciences in Washington.
Pregnancy, menopause or polycystic ovarian syndrome (a hormonal disorder) can cause cysts to appear, as can other triggers that change hormonal levels, such as stress or birth control use.
Other factors
Cystic acne is not exclusively caused by hormones. Environmental factors such as high humidity and excessive sweating may play a role, in addition to cosmetics, cleansers, lotions, and clothing that traps sweat.
Genetics are a contributing factor; if one of your parents had cystic acne, unfortunately you are more likely to develop it as well.
Specific drugs and chemicals can also contribute to the development of cystic acne or cause existing breakouts to worsen. Compounds that are known to be problematic include corticosteroids, lithium, phenytoin, and isoniazid.
While the link between acne and diet hasn’t yet been fully established by research, some people find that reducing or eliminating their consumption of dairy greatly reduces the occurrence of cystic acne. However, the American Academy of Dermatology (AAD) reports that existing evidence is not strong enough to support this theory.
High glycemic foods and lack of exercise and sleep have also been linked to acne.
What is the best cystic acne medication?
Unlike mild forms of acne, it is not advisable to wait out cystic acne to see if it will resolve on its own. Waiting will increase the odds that the cysts will leave behind a severe scar when they finally do heal.
Isotretinoin
Isotretinoin is a medication primarily used to treat severe acne. More commonly known by its brand name Accutane, this drug was discontinued in the United States in 2009. However, there are plenty of generics available on the market, all derived from vitamin A, that have been shown to treat acne when taken orally.
“Isotretinoin or Accutane is our standard of care for severe recalcitrant cystic acne,” said Dr. Bobby Buka, the founder of Bobby Buka MD Dermatology in New York City. “We’ll prescribe these medications when scarring is getting worse and worse. Cystic acne is particularly nefarious because it can lead to permanent scarring if not treated speedily.”
Isotretinoin has been shown to be safe and effective in reducing scar-prone acne.
Oral antibiotics
While antibiotics can’t reduce excess oil or get rid of dead skin cells, they can decrease bacteria and inflammation that contribute to cystic acne.
Your dermatologist will likely prescribe a short course of antibiotics to reduce your chances of developing bacterial resistance.
“I’ll usually start patients with an oral antibiotic like minocycline or doxycycline. If these don’t work, then we go up from there,” Dr. Buka notes.
Topical retinoids
These products are derived from the same ingredient as isotretinoin—vitamin A. Topical retinoids unclog hair follicles and help prevent acne from forming. Retinoids come in many forms, including cream, gels, and lotions.
Skin may redden and peel as it adjusts to the new product, and retinoids often increase skin’s sensitivity to the sun. It is recommended to be extra-vigilant about wearing sunscreen while using topical retinoids.
Spironolactone
This oral medication is generally used to treat high blood pressure and swelling. However, it’s also been found to be an effective treatment for acne—including cystic acne—particularly for women who have acne around their jawline or lower face.
Oral contraceptives
Oral contraceptives contain estrogen that help regulate hormones—and acne that may be caused by hormone fluctuations.
If you tend to develop cysts at specific times during your menstrual cycle, you should ask your doctor about birth control pills, if you’re not already taking them. However, it is important to weigh the risks of taking oral contraceptives against the potential benefits you may derive from doing so.
Corticosteroid injections
If you have a skin emergency— perhaps a major cyst appears before a big presentation—you can try having a corticosteroid injection.
Your dermatologist will inject the site—the cyst may be drained beforehand. The cyst will start to reduce in size within a few hours and usually disappears in about a day.
Bear in mind that these injections have been known to lead to scarring and/or hyperpigmentation, especially with repeated use. Only turn to this procedure when you absolutely have to.
» Learn more about the differences between whiteheads and blackheads, and how the treatments differ
How to prevent cystic acne
While there’s no single foolproof way to guarantee you’ll never have a cyst again, adopting a combination of preventative approaches can greatly reduce your chances.
- Never go to bed with makeup on, as this can clog pores and lead to breakouts.
- Select noncomedogenic, oil-free makeup that will be less likely to clog your pores.
- Wash your skin immediately after exercise or sweating to reduce bacteria.
- Wash your hair regularly if your scalp tends to be oily; if your hair is in contact with your face, the oil can lead to clogged pores.
- For men, use caution when shaving and ensure you lather up well to avoid irritating skin.
“Eating a balanced diet, minimizing stress, exercise, sleep—all will keep inflammation to a minimum,” Dr. Friedman explains. “This won’t get rid of all acne, but doing the opposite— eating foods that are high on the glycemic index, poor sleep habits, stress—will all worsen acne.”
When should I see a dermatologist?
Cystic acne can be both emotionally and physically scarring, and the longer you wait, the more likely it is that your cystic acne will scar.
If you notice a cyst developing, don’t hesitate to schedule an appointment with your dermatologist to discuss the treatment option that is right for you. In the meanwhile, follow these common sense skincare tips:
- Don’t pop cysts or pick at them; this can cause scarring or spread the inflammation.
- Use a gentle cleanser to avoid irritating your breakouts further.
- Avoid harsh exfoliants and excessive washing, as this can dry out skin.
» To learn more about cystic acne treatments, meet our Medical Review Team.