- The exact cause of diabetic dermopathy is unknown, although it’s been linked to a variety of diabetic complications.
- Despite the link between the two conditions, you don’t have to have diabetes to get diabetic dermopathy.
- Diabetic dermopathy may be easily confused for similar looking skin diseases, so be sure to seek out a professional diagnosis.
- Although the condition often clears up on its own, you should still see a doctor if you think you have it.
What is diabetic dermopathy?
Diabetic dermopathy goes by many names: shin spots, sugar spots, and even spotted leg syndrome. This relatively innocuous skin condition may not be particularly dangerous on its own. At the same time, it could indicate some serious underlying medical conditions, which is all the more reason to know if you’re at risk, how you can spot it, and when you should consult a physician.
What does diabetic dermopathy look like?
When you first notice there’s a problem on your skin, it will look like scaly red or purple patches. These patches will be circular in shape and may vary in size. They won’t blanche when you press them. In other words, your skin would normally turn temporarily white when you press it hard with a finger or thumb, but these patches won’t change color in response to similar pressure.
In some cases these patches could be raised or swollen. They could take on a pimple-like appearance (papules). In other cases, they could be flat (macules). However they first appear, they’ll eventually give way to the more recognizable form of the condition.
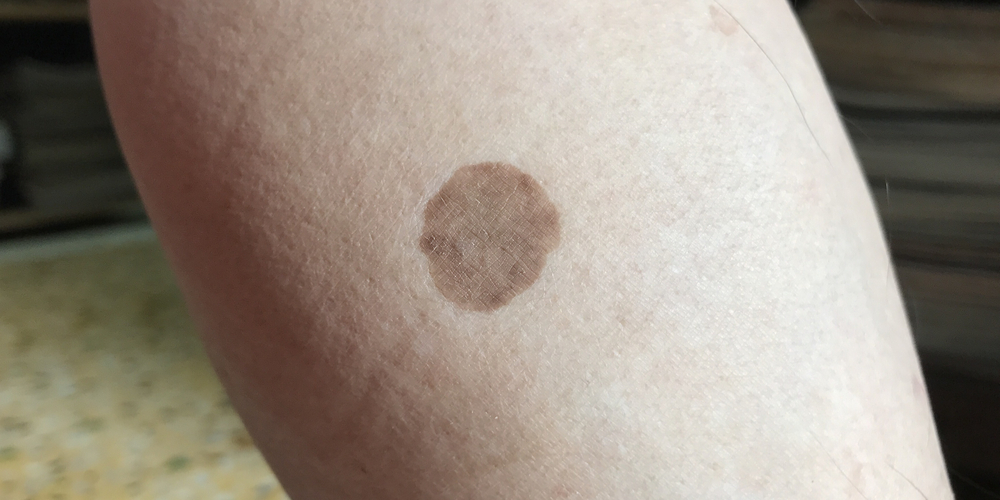
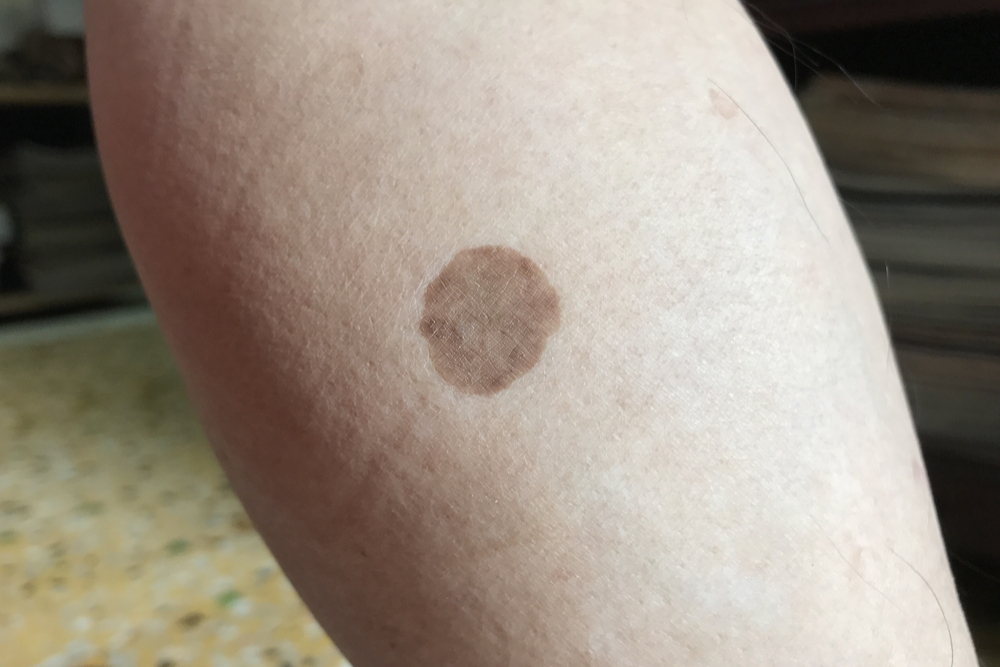
Eventually, these scaly patches flatten out even more. These spots (and sometimes lines) may maintain some of their reddish hue, or they could turn to light or dark brown patches. They also take on a shiny appearance. Finally, these spots can atrophy, causing them to have a weakened and even indented appearance. It’s said that spots with greater degrees of atrophy are also darker.
Diabetic dermopathy spots are small, typically only a centimeter in diameter, though some longer spots can grow to 2.5 cm in length. They may be unsightly, but they’re usually asymptomatic.
» Do you have spots that you suspect might be diabetic dermopathy? Meet our medical review team to address your concerns and get appropriate recommendations.
What symptoms should I look for?
At first, the spots may feel scaly, but they’ll eventually become soft. You may be able to feel an indentation in your skin if you lightly rub a finger over a spot, a result of the atrophy. Most diabetic dermopathy spots don’t come with any other symptoms, but some people have found them itchy or have felt a burning sensation. If this happens, you should avoid scratching them. Nevertheless, be reassured that in either case they are generally harmless.
Where do these spots occur?
Diabetic dermopathy most frequently appears on the shins, hence the nickname “shin spots.” However, you might also see it on your arms, feet, thighs, or torso. These spots appear to be more common in bony parts of the body, which is one reason why they appear so frequently on the shins.
» If you’re interested in learning more about what to expect with diabetic dermopathy, discuss with our medical review team for more information.
Who is at risk for diabetic dermopathy?
Diabetic dermopathy is most common in people with diabetes, especially older patients who have been diabetic for around 10–20 years. It’s unclear exactly how common the condition is among those with diabetes, with an estimated incidence rating between 9% and 55% in general and around 40% among diabetic patients over 50. In any case, it is considered the most common skin condition associated with diabetes.
Although those without diabetes are sometimes diagnosed with diabetic dermopathy, the correlation between the two diseases is so strong that it’s highly recommended that anyone who notices these spots get checked for diabetes. This is especially true if you have four or more lesions, as this only occurs in diabetic patients.
Finally, these spots are also more common among people with certain diabetic complications like retinal damage or disease (retinopathy), nerve damage (neuropathy), or kidney damage (nephropathy), suggesting that they may have a common cause.
What causes diabetic dermopathy?
It’s unclear why exactly these spots occur, though researchers and medical professionals do have some theories. Given its relationship to diabetes, it’s thought to have something to do with changes in blood sugar levels or in the small blood vessels themselves that supply the skin. A 2004 study observed reduced blood flow in areas of the body affected by diabetic dermopathy.
Shin spots have also been observed to occur in response to extreme temperatures or mild blunt-force trauma. It’s thought that the spots themselves could be the body’s overreaction to injury. The fact that they occur on bonier parts of the body lends credence to this idea.
Are there any risks associated with diabetic dermopathy?
On its own, the skin condition is innocuous. As we mentioned above, some report mild itchiness or burning, but most people don’t experience any symptoms other than the spots themselves. That being said, it’s still important to see your physician if you notice the spots.
First of all, you want to be sure they aren’t indicative of more serious skin disorders. Your physician can perform a differential diagnosis, eliminating the possibility that you might have another condition that looks similar to diabetic dermopathy. During this time, you also want to be checked for diabetes, if you’ve not already been diagnosed with it.
Finally, given the correlation between diabetic dermopathy and other diabetes complications, you want to be checked out for retinal, nerve, or kidney damage. Some research even suggests that there could be a correlation between diabetic dermopathy and heart disease.
» Do you have diabetic dermopathy? Discuss with our medical review team for an official diagnosis and to get checked out for diabetes.
Does diabetic dermopathy resemble any other conditions?
Because diabetic dermopathy is usually symptom free, it’s frequently confused with age spots, also known as liver spots, which have a similar appearance. It is also sometimes confused with pigmented purpuric dermatosis, also known as capillaritis, which involves similar dark spots that tend to affect the legs. Finally, differential diagnoses will rule out stasis dermatitis, an inflammatory disease, and necrobiosis lipoidica lesions, both of which also tend to appear on the legs.
Diabetic Dermopathy is also easily confused with venous insufficiency. Although the latter is not a skin condition, it can lead to dark spots on the legs due to faulty or poor drainage in the veins. This darkening tends to start near the insides of the ankles and spread from there. Although it’s true that some medical experts attribute diabetic dermopathy to changes in vessels that supply the skin, that’s not the same as venous insufficiency, which affects a larger area and is often painful.
When diagnosing diabetic dermopathy, physicians look for diabetes. That tends to be a determining factor. You could however still receive a diagnosis of diabetic dermopathy even without having diabetes if these other conditions are ruled out.
How is diabetic dermopathy treated?
Diabetic dermopathy should go away in time, even without medical care. The spots typically start to fade between 18 months and two years after first appearing, but they could stick around indefinitely. Without knowing what exactly causes them, it’s difficult for medical professionals to say for certain when they’ll disappear.
There is no treatment for diabetic dermopathy that will make the spots fade faster. However, if you are experiencing uncomfortable symptoms, there may be a topical over-the-counter or prescription cream that can help you. As with most itchy skin conditions, you should avoid scratching the area for fear of causing skin damage that could lead to scarring. Itching could also bring about infection and extend the length of time before your skin returns to normal.
Finally, if you are diabetic, take this as a sign that you might need to take better control over your condition. Of course, without knowing exactly how they are caused, it’s hard to predict what will help. If the spots are indeed linked to blood glucose levels, it’s possible that you need to be more careful about monitoring your insulin levels and watching your diet. Whatever their cause, talk to your doctor about what you can do to improve your diabetes management.