- Folliculitis is a common benign skin condition caused by the presence of inflammatory cells within the hair follicle
- While not life threatening to most, folliculitis can cause discomfort, and be aesthetically unappealing.
- Certain at-home remedies can be helpful in treating folliculitis
- Simple actions like regular bathing, particularly after exercising, significantly reduce the chances of acquiring folliculitis
What is folliculitis?
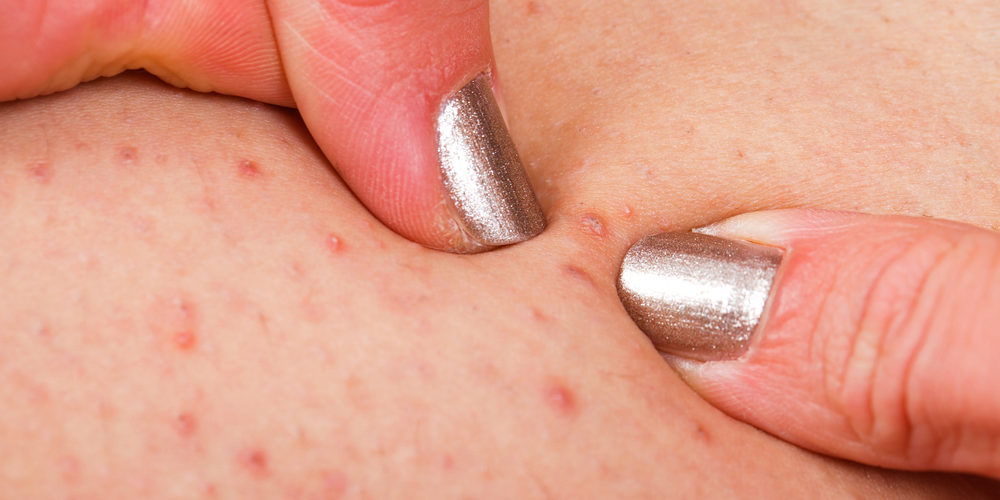
Folliculitis is a common benign skin condition caused by the presence of inflammatory cells within the hair follicle. These cells create a red bump or acne-like pustule.
Inflamed hair follicles, typically infected by the bacteria staphylococcus aureus, result in rashes, itchy skin, swelling, and small white pimples with varying degrees of redness in the affected area. While bacteria causes many cases of folliculitis, fungal, viral, and non-microbial varieties of folliculitis also exist.
What causes folliculitis?
Fungal folliculitis is commonly caused by yeast, while viral folliculitis occurs when the herpes virus spreads to hair follicles, usually around the mouth.
Non-microbial folliculitis combines multiple types of the condition. These include pseudofolliculitis barbae, caused by hair curling back under the skin, folliculitis decalvans, caused by multiple hairs growing out of the same hair follicle, and oil folliculitis, caused by exposure to certain oils.
As the condition is tied to hair follicles, folliculitis can occur anywhere on the body where hair can grow, but is typically found on the arms, back, legs, and in the beard area.
Is folliculitis dangerous?
While not life threatening to most, folliculitis can cause discomfort, and be aesthetically unappealing. However, in certain cases folliculitis can have serious repercussions.
“In those with a weakened immune system, folliculitis can have more severe consequences and may lead to blood stream infections, but this would be extremely rare,” says Dr. Mercedes E. Gonzalez, Medical Director at Pediatric Dermatology of Miami.
Folliculitis can subside on its own without treatment, but it can also worsen over time if left untreated. “Folliculitis can be dangerous, and can spread if it is caused by bacterial infection,” says Dr. Purvisha Patel, a cosmetic surgeon and dermatologist at the Advanced Dermatology & Skin Cancer Associates in Memphis. “It can be hard to treat if caused by a fungus.”
While more severe cases may cause permanent hair loss or scarring, in most cases medication or over-the-counter treatments produce rapid results.
Home treatments that work — and those that don’t
While both Gonzalez and Patel agree that seeing a professional dermatologist is ideal when managing folliculitis, some might opt for a home remedy. Whether due to time or financial constraints, choosing to treat folliculitis at home has its clear advantages, but it also holds the risk of undesirable outcomes.
That being said, out of the various home remedies described online, Patel and Gonzalez have seen many that do nothing, some that could worsen the condition, and even a few that could cure it.
At-home treatments that work
Certain at-home treatments take advantage of everyday items’ antiseptic, or anti-inflammatory qualities. Applying white vinegar, neem leaves, garlic, or turmeric can help lessen the effects of bacterial folliculitis, and in some cases cure it.
Other purported cures, such as applying oatmeal, can help to manage discomfort. However, this is unlikely to solve the underlying issue.
Patel and Gonzalez suggest their own variations on home treatment.“I would recommend benzoyl peroxide wash, witch hazel, and antibacterial soaps,” says Gonzalez. For her part, Patel recommends applying tea tree oil to help with bacterial and fungal folliculitis.
Many who are afflicted by folliculitis require treatment on a reoccurring basis, as the condition tends to resurface on susceptible people. Managing this form of repeat folliculitis calls for its own form of treatment.
“Since it can be a problem that comes and goes in people who are prone to it, using an antibacterial wash daily can help prevent recurrence,” says Gonzalez.
Home treatments to avoid
Patel and Gonzalez both agree that oily home treatments should generally be avoided. Coconut oil and body lotion are two commonly reported remedies that may do more harm than good.
While they might help to mildly soothe non-microbial folliculitis, these oily agents can block up pores, and can even worsen microbial varieties of folliculitis.
Antibiotics may be the clear choice for many, but Gonzalez urges a certain level of caution. “Applying over the counter antibiotics should help with folliculitis, but an ointment base can trigger the clogging of pores and hair follicles, which can lead to more folliculitis,” says Gonzalez.
Preventing folliculitis
Although treatment is important, prevention can literally stop the problem at its root. Simple actions like regular bathing, particularly after exercising, significantly reduce the chances of acquiring folliculitis. Sharing facecloths and towels should be avoided when possible.
Hot tub folliculitis
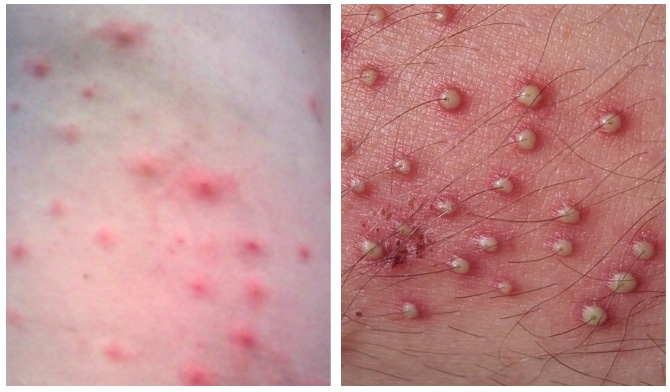
Hot tub folliculitis typically appears across large sections of the body, and can easily be mistaken for chickenpox, especially when considering that this form of folliculitis often impacts children.
The red marks present on the body tend to itch, or even burn. With minimal scratching, the itchiness and marks should subside without further treatment in roughly two weeks, leaving darkened patches of skin behind. These dark patches can take several months to fade.
The bacterium responsible for this skin condition, pseudomonas aeruginosa, thrives in shared watery spaces like water parks or public pools that do not meet cleanliness standards. Avoiding areas such as this or showering following swimming is crucial to prevention.
Razor bumps
Pseudofolliculitis barbae, a non-microbial variety of folliculitis, is also known as “razor bumps,” as shaving or plucking hair can cause the inflammation to occur. As both involve a level of discomfort and redness following shaving, some confuse razor bumps with razor burn, however the two are distinct conditions.
Razor burn tends to fade quickly following shaving, and is only the result of a skin irritation. Razor bumps last longer than razor burn, and tend to have a more prevalent redness that also includes the characteristic small white pimples of folliculitis.
If the early signs of pseudofolliculitis barbae and other varieties of folliculitis do appear, it is important not to scratch impacted areas. While itchy, scratching and shaving can spread and worsen cases of folliculitis. This early stage would also be the key time to seek out a dermatologist if possible, and switch to an antibacterial soap.
Pityrosporum (malassezia) folliculitis
According to Marjorie Mahone, creator of a blog dedicated to this little known skin condition, pityrosporum (malassezia) folliculitis is often misdiagnosed as acne, primarily because an acne-like eruption presents itself on the skin. For this reason, pityrosporum folliculitis is typically only discovered after months and sometimes years of unsuccessfully treating what is thought to be acne.
The yeast at the root of pityrosporum folliculitis is malassezia, which is commonly found on skin and is generally harmless. However, under the right conditions, malassezia can overgrow and cause a fungal infection of the skin. This overgrowth can ultimately lead to the presence of tiny, acne-like papules and pustules, and the occasional itch at the site of infection.
Keeping yourself cool and dry, showering after exercising and sweating, wearing loose, breathable clothing, and spending less time in hot and humid environments may help in preventing pityrosporum folliculitis.
It is also best to avoid applying greasy and oily products to the skin and hair, and to limit the use of antibiotics and steroid medications unless deemed necessary. In general, boosting the immune system, maintaining a healthy diet and taking a daily probiotic are key to preventing pityrosporum folliculitis, which is known to recur.
Final words of advice
While home cures and prevention are often the cheapest and most accessible solution when managing folliculitis, more drastic solutions are available when necessary or desired. As the condition goes untreated, or improperly treated, it can cause additional discomfort and even pain.
“If there are large folliculitis bumps, sometimes that can be painful, so you can inject intralesional triamcinolone [an injectable cortisone] to the larger lesions,” says Gonzalez, “this will provide pain relief and decrease inflammation.”
The key element to successful home treatment is determining the underlying cause of the issue. What might help to treat non-microbial folliculitis, for example, may worsen cases of bacterial folliculitis. Distinguishing between the types can be difficult to the untrained eye.
As few who attempt self-managing folliculitis have the skill set of a dermatologist, “home treatment may worsen the problem, or even cause their own separate problems, such as allergic or irritant contact,” warns Gonzalez.
At-Home Treatments for Folliculitis: Top Products

While at-home remedies are no substitute for professional help, more mild cases of folliculitis may be entirely treated at home. Your success with any home remedy will depend on the causes and type of folliculitis you’re dealing with. The following treatment options are in line with expert dermatologists’ suggestions.
Ovante Folliculit Solution Body Lotion
The herbal extracts effectively work against mild to chronic folliculitis and other skin-related problems, relieving you from any irritation and itching. Regular use reduces the chances of new skin breakouts.
CLn Scalp Shampoo
This unscented shampoo cleanses the hair and flaky scalp effectively, including dandruff, itching, redness, and folliculitis, giving you healthy-looking hair and scalp. The formula works gently on your beard and after shaving.
Hibiclens – Antiseptic/Antimicrobial Skin Cleanser
The active ingredients help kill harmful bacteria, viruses, and fungi. This antiseptic liquid soap offers protection of about 6 hours against any infections that you may come in contact with and also eliminates the risk of transfer.
CLn Non-Drying BodyWash
This dermatologist-tested product effectively reduces skin dryness, redness and flakiness caused due to eczema, folliculitis, and various other skin conditions. It gently cleanses the affected areas of the skin and promotes healthy skin. Free of harsh chemicals.
DRMTLGY Exfoliating Body Lotion
This body lotion is a blend of Alpha Hydroxy acids that aids in relieving many skin conditions, including Keratosis Pilaris and folliculitis. This unscented moisturizer will give you soft and smooth skin as well as relieve flakiness and redness.