- Granuloma annulare is noncancerous, noncontagious condition that causes ring-shaped patches on the skin.
- It is often mistaken for ringworm and other common skin disorders.
- Granuloma annulare usually resolves on its own, but severe forms may require treatment.
Found in patients of all ages, granuloma annulare is a common and benign skin condition that produces ring-shaped lesions, generally on the hands and feet. Its exact causes are unknown.
Although there is no known cure for granuloma annulare and it generally self-resolves, dermatologists may recommend various treatments to alleviate its symptoms.
What are the symptoms of granuloma annulare?
Granuloma annulare (GA), also known as necrobiotic papulosis, is a relatively common and noncontagious condition that produces smooth, thick patches on the skin.
These raised patches are often discolored and scaly, forming rings (annulare is Latin for “ring-shaped”) that can be found anywhere on the body, although the arms, legs, hands and feet are often more severely affected. For these reasons, it is sometimes mistaken for ringworm.
At times, GA occurs in patients who also suffer from a similar condition called necrobiosis lipoidica. This condition is associated with diabetes and rheumatoid arthritis, whereby skin cells die from necrosis and are not replaced.
While GA usually does not itch or burn, individuals may experience pain when the patch is touched or irritated through contact. In some cases, round lumps may develop on the skin instead of the ring-shaped plaques. These may also cause pain when irritated.
Young girls and young adults of both sexes are the most commonly affected, but since it arises from an immune response, anyone can develop granuloma annulare.
Granuloma annulare and the immune system
The exact mechanism by which GA forms continues to be researched. What science currently understands is that this skin condition is caused by a delayed hypersensitivity reaction (i.e., an allergy) in response to an aggravation in a specific layer of the skin called the dermis. This may be triggered by an animal or insect bite, minor skin lesions, sun exposure, a tuberculin skin test or vaccination.
After one of these events, the immune system launches an inflammatory response via a signal called tumor necrosis factor alpha, or TNFα, which activates a number of other processes in the body and leaves behind plaques in those regions. This inflammatory response is a normal reaction intended to fight infection and prevent disease.
Case reports show that for the most part, healthy people develop GA. However, individuals living with certain chronic illnesses are at greater risk.
These illnesses include:
- Autoimmune thyroiditis (a thyroid disease)
- Bacterial infections
- Diabetes mellitus
- Herpes zoster virus (shingles)
- Human immunodeficiency virus (HIV)
- Hyperlipidemia (high cholesterol)
- Lymphoma (cancer of the immune system)
- Solid tumors
The six subclasses of granuloma annulare
Even though GA produces characteristic annular plaques, the distribution patterns, locations of these plaques, and the ages of those affected can be separated into six sub-classes: generalized, subcutaneous, localized, interstitial, atypical, and perforating.
- Generalized
Generalized GA primarily affects adults, with patches or small papules that range in color from the person’s normal skin tone to pink or mauve. These patches are often symmetrical rings with diameters of 10 cm or more. Areas affected are skin folds such as the armpits and groin.
- Subcutaneous
Subcutaneous granuloma annulare is seen exclusively in children, causing rubbery lumps to develop on the skin.
Because they are often found in the same areas as the nodules seen in people with rheumatoid arthritis — on the fingertips, shins, and along the edges of the scalp — these lumps are sometimes referred to as pseudo-rheumatoid nodules.
- Localized
Localized GA, the most common type of GA in children, presents as one or multiple raised, round, ring-like patches that may appear singly or coalesce into groups of ring-like patches in the skin overlying joints. The center of each patch is usually recessed.
Affected areas are the joints of hands and fingers, elbows, and the tops of feet and ankles.
- Interstitial
Interstitial granuloma annulare, also referred to as interstitial granulomatous dermatitis, describes more widespread plaques or papules covering significant areas of the trunk — especially on the back — that cause bouts of itching and burning sensations. These plaques are not always annular, and may take on a round or cord-like distribution.
Middle-aged women living with autoimmune disease experience this form of GA the most.
- Atypical
Atypical GA, as its name implies, is unusual in its higher level of severity and uncharacteristic trait of developing after exposure to sunlight. It affects smaller, more uncommon areas of the body such as the palms of hands, ears, and face.
- Perforating
Perforating GA is a rare subset that typically itches and is tender to the touch. Found in all age groups, large plaques form by pushing damaged collagen through the surface layer of the skin.
These large annular plaques appear anywhere on the body, but they tend to favor the hands. This form is most likely to leave scars.
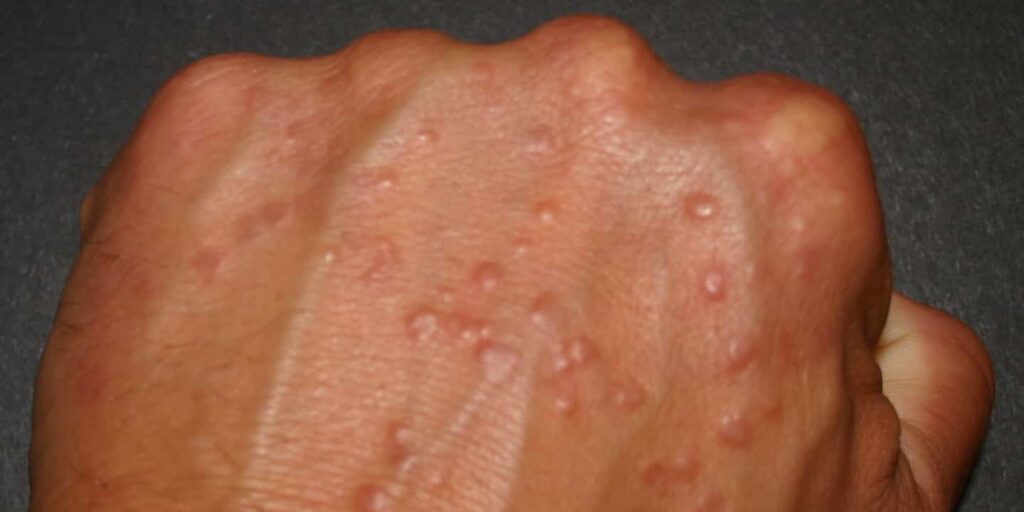
Granuloma annulare treatment options
Treatment is not required in all cases, as GA almost always resolves on its own and is not contagious. It can take anywhere from a few months to several years for the plaques to disappear, but the average period is two years.
Nevertheless, some individuals make the decision to pursue treatment if they feel that it affects their quality of life. The following treatment options are available through a healthcare provider or dermatologist:
- Topical corticosteroids or topical steroids reduce inflammation and the appearance of plaques.
- Corticosteroid injections are as effective as topical corticosteroids, but work more rapidly as they are directly injected into the affected skin.
- Cryotherapy destroys plaques by freezing the affected skin.
- Malaria drugs such as chloroquine and hydroxychloroquine are very effective for GA forms that are more widespread or present in a deep nodule, but take about three months to be effective.
- Combination therapy using minocycline, rifampin, and ofloxacin, has been effective in treating individuals that do not respond to other treatments.
- Fumaric acid in low doses has been shown to improve and even remove GA patches.
- Light therapy or photodynamic therapy is reserved for more invasive GA, and alleviates patches by exposing affected skin to ultraviolet rays.
- PUVA therapy or photochemotherapy takes light therapy a step further by combining psoralen (P) to make skin more sensitive to light therapy, and then exposing patients’ affected areas to ultraviolet A (UVA) rays.
- Antibiotics can help facilitate any of these treatments by killing bacterial infections that may have initially caused the skin condition.
It is important to note that some of these treatments have side effects, such as nausea and hyperpigmentation. Ultraviolet A therapy is known to cause burning, photo-aging, and an increased risk of skin cancer.
When should I see a dermatologist?
Dr. Debra Jaliman, author of the book Skin Rules: Trade Secrets from a Top New York Dermatologist, states that many times granuloma annulare will go away on its own.
“Your physician may prescribe corticosteroid topical creams for GA,” Jaliman says. “This will help improve the appearance of the lesions.”
The American Academy of Dermatology (AAD) also recommends that individuals see a dermatologist to determine their skin condition and receive the proper treatment. Furthermore, the AAD encourages people living with GA to remain patient while waiting for patches to clear, but to be watchful of any itching or tenderness that may develop.
Also be aware there is also the possibility of GA returning once it does resolve. Schedule follow-up visits with your dermatologist to monitor your condition.
» To find out more about granuloma annulare, use Zwivel’s online consultation tool to contact a board-certified dermatologist in your area.