- Although the exact causes remain unknown, scientists believe that lupus develops from a combination of internal and external factors.
- Symptoms of lupus can vary depending on patients, which makes diagnosis difficult.
- An official list of 11 criteria has been established for diagnosing Systemic lupus erythematosus (SLE).
What is lupus?
Lupus — also known as Systemic lupus erythematosus (SLE) — is a chronic, systemic, autoimmune, inflammatory disease. The body’s immune system attacks healthy tissues and organs, notably the skin, joints, heart, blood vessels, brain, kidneys, bones and lungs.
Typically, our immune system makes antibodies to fight against foreign invaders like viruses and bacteria. However, in the case of lupus, the immune system makes antibodies that attack the body’s healthy tissues. These antibodies, called autoantibodies, attack various parts of a person’s own body, causing pain, inflammation and damage.
“Chronic” means the disease is lifelong. Symptoms such as skin rash and fatigue may come and go, but the underlying condition of lupus will remain. “Systemic” signifies that lupus affects many parts of the body, while “autoimmune” means the body’s immune system is attacking its own tissues.
Lastly, “inflammatory” indicates that the body responds the way it would to an infection or injury – with swelling, heat, pain and redness.
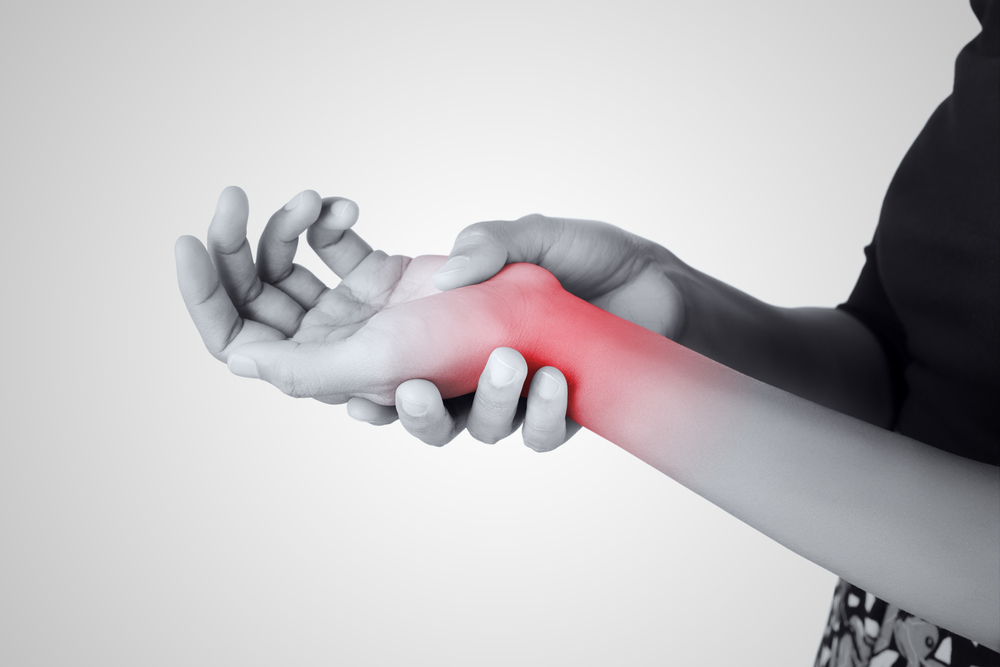
What are the symptoms of lupus?
- Tiredness or fatigue
- High fever
- Weight loss
- Hair loss
- Pain in the chest when breathing
- Nose, mouth, or throat sores
- Sensitive to sunlight
- Muscle aches
- Joint pain
- Poor circulation in fingers and toes
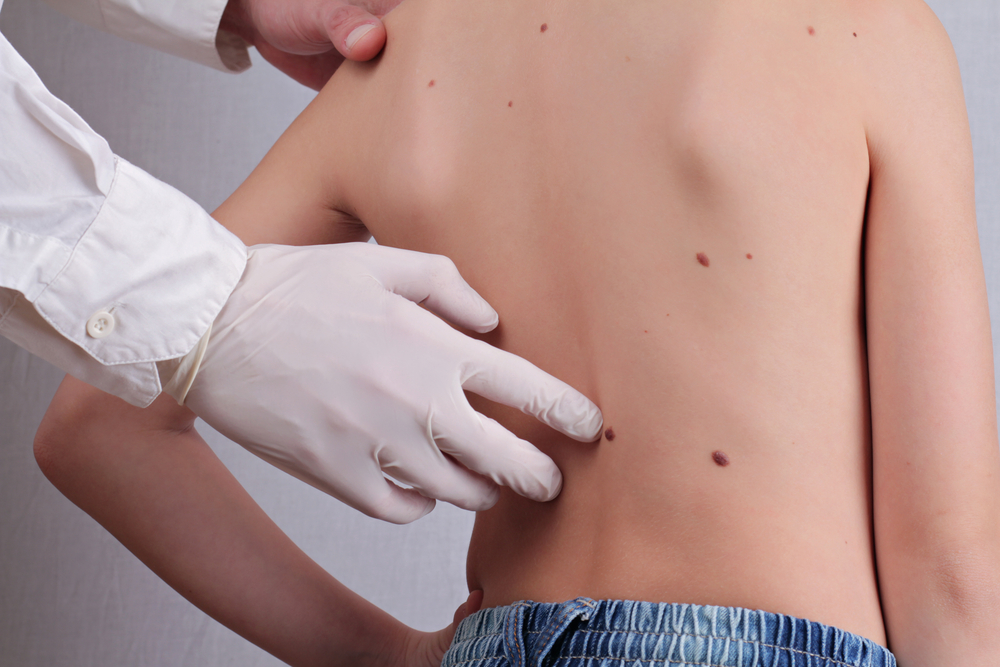
- Skin rash
- Dizziness and headaches
What are the causes of lupus?
Although scientists do not all agree, many believe that lupus develops from a combination of factors inside and outside the body. The theory is that the condition is essentially caused by a mix of hormones, genetics and environment.
More women have lupus, and their symptoms usually appear at times when estrogen levels in the body are high, such as before periods or during pregnancy. However, no causal link between estrogen or any other hormone and lupus has been proven.
Researchers have identified over 50 genes associated with lupus. They are not believed to cause lupus directly but may contribute to it in the presence of other factors, including environmental triggers. The most commonly suspected triggers include:
- Ultraviolet light (UVA and UVB)
- Infections (especially Epstein-Barr virus)
- Exposure to silica dust in agricultural or industrial settings
- Certain antibiotics
- Emotional stress
How is lupus diagnosed?
Dr. Maral Skelsey, director of the Dermatologic Surgery Center of Washington in Chevy Chase, MD says, “Lupus mainly affects women and the skin is involved in 80% of patients. Four of the 11 criteria for lupus involve the skin and mucous membranes.”
The American College of Rheumatology has made an official list of 11 criteria for diagnosing SLE. At least four or more criteria need to be met before making a possible lupus diagnosis. The 11 criteria are:
- Butterfly-shaped rash across the cheeks and nose (called a malar rash)
- Raised red patches on the skin (called a discoid rash)
- Unusual skin reaction to sunlight (photosensitivity rash)
- Typically painless mouth or nose ulcers
- Arthritis in two or more joints – without evidence of bone erosion but with tenderness, swelling, or fluid buildup
- Inflammation of the lining around the heart (pericarditis) and/or lungs (pleuritis)
- Excessive protein in the urine
- Low red blood cell, white blood cell or platelet counts
- Specific antibodies to double stranded DNA, Smith (or Sm) antigens or cardiolipin
- A positive test for antinuclear antibodies (ANA) – however, a positive ANA test does not necessarily mean someone has lupus
- Seizures or psychosis (neurologic symptoms)
If multiple criteria are present simultaneously, the specialist may diagnose lupus, but often symptoms gradually appear over time so the diagnosis may not be immediately obvious.
Why is lupus so hard to diagnose?
When lupus is suspected, your doctor will look for signs of inflammation in the body, which can occur visibly outside on the skin or inside internal organs, like the kidney or heart. The latter signs cannot be seen visually but may be detected using diagnostic tests and/or imaging. Signs of inflammation include pain, heat, redness, swelling and loss of organ function.
Doctors have given lupus the nickname “the great imitator” because its symptoms can be confused with many other illnesses. Symptoms vary from person to person, come and go, and often change over the course of the disease. It can sometimes take several years to reach a lupus diagnosis. Keeping track of symptoms and consulting a rheumatologist may help sufferers get an earlier diagnosis.
Unfortunately, no laboratory tests can provide a definite “lupus” or “no lupus” diagnosis as the same lab results may be found in people with other illnesses. Also, different labs produce different results that may change – it may be positive one time and negative the next.
At what age can a clear diagnosis be reached?
Only 15% of people with lupus have symptoms before the age of 18 years. Symptoms usually emerge between the ages of 15 and 44 years. Also, women are much more likely to develop lupus than men. Children diagnosed with lupus will be referred to a pediatric rheumatologist.
How is lupus treated?
Most people are primarily followed by a rheumatologist but since lupus affects many other organ systems as well, consultations with other specialists are often needed, including dermatologists, cardiologists, nephrologists and neurologist.
“Medications used to treat lupus target the systems involved,” explains Dr. Ronda Q. Klein, a board-certified dermatologist in Westport, CT. “NSAIDS and corticosteroids are often used initially given their quick onset and alleviation of joint pains and systemic disease. Patients are then transitioned to non-steroidal disease-modifying agents, such as anti-metabolites (azathioprine, methotrexate, cyclosporine), antimalarials and mycophenolate to prevent further damage, cytotoxic drugs (cyclophosphamide), and rituximab,” she notes.
In 2011, the first new drug in 50 years, belimumab, was FDA approved for lupus. Belimumab is a monoclonal antibody that targets the B-lymphocyte stimulator protein, BLyS, which reduces disease activity. This new drug falls into the biologic category of medications and they generally end with the suffix “mab.”
Biologic therapies have been developed to treat psoriasis, rheumatoid arthritis and other autoimmune diseases. “Biologic therapy is also being used off-label for SLE,” explains Dr. Klein.
With current new treatments, the periods of remission from lupus may last several years. This offers hope that research will someday lead to even better treatments and eventually a cure.
Is there more than one kind of lupus?
While there are different types of lupus, systemic lupus erythematosus (SLE) is the most common and serious form.
Drug-induced lupus (DIL) has many of the symptoms of SLE, but it goes away once the medication is stopped. Over thirty medications have been associated with cases of DIL, the three most common being hydralazine, a blood pressure medication; procainamide for heart arrhythmias; and isoniazide, an antibiotic for treating tuberculosis.
Discoid lupus erythematosus (DLE) and subacute cutaneous lupus erythematosus (SCLE) are diseases that affect the skin but do not involve the internal organs.
Lastly, neonatal lupus can occur in newborns whose mothers have SLE. In neonatal forms of this condition, skin lesions develop during the first weeks of life. These lesions are usually harmless and disappear with time as the baby ages.
Is lupus contagious, cancerous, or hereditary?
Lupus in not an infection. It cannot be passed from person to person like a cold or the flu. Lupus is also not a type of cancer. As treatment options improve, many patients experience periods with no symptoms, called remission. Although we often hear the word “remission” in association with cancer, this does not mean that these diseases are synonymous.
Sometimes people with lupus have one or more family members with lupus or an autoimmune disease. Although genes associated with lupus have been found, these markers are not thought to directly cause lupus but rather contribute to it indirectly.
Can lupus be fatal?
Kidney failure used to be the leading cause of death with lupus. However, better treatments, access to dialysis and the possibility of kidney transplants has lowered the death rate due to kidney failure.
Currently, cardiovascular disease is the leading cause of early mortality in people with lupus. It is especially important for people with lupus to minimize risk factors for heart disease. These actions include lowering cholesterol, not smoking, maintaining a healthy weight and getting regular exercise.