- Milia can affect anyone, from newborn babies to elderly patients.
- There are many potential causes of milia, which can often be traced to your skin-care regimen or a separate issue that has affected the surface of the skin.
- Thick creams and makeups should be avoided if you’re looking to prevent milia
What are milia?
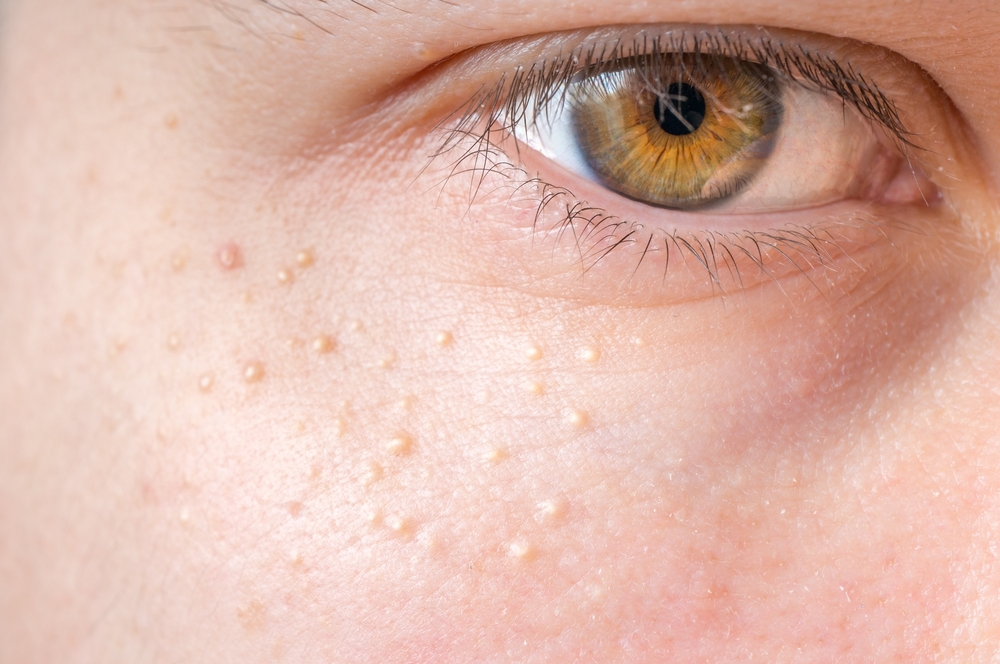
Also referred to by the terms milia cysts, milia bumps, and “milia acne” ( even though it’s not acne), these benign, bead-like cysts can be incredibly bothersome, especially if they keep coming back no matter how clean you keep your skin.
Milia do not form due to a lack of cleanliness. Usually, the issue is the skin’s inability to properly exfoliate, which happens as a result of skin cells becoming trapped beneath the skin’s surface.
Milia usually appear on the face, but can also occur on the mucous membranes in the mouth (cheek) or lips. The areas that are most commonly affected are the eyelids, lips, forehead, arms, and hands.
Milia can affect anyone, from newborn babies to elderly patients. Sometimes they disappear as the surface layer of skin wears away, but in many cases they will remain over long periods of time.
If milia don’t go away on their own, meet our medical review team.
What causes milia?
There are many potential causes of milia, which can often be traced to your skin-care regimen or a separate issue that has affected the surface of the skin.
Here are some of the most common culprits:
Use of heavy skin care products
The most common cause of adult milia is use of heavy skin and hair care products and items. Comedogenic products — those containing oils — can interfere with the skin’s ability to shed dead skin cells.
Products fitting this description can include comedogenic makeup remover, moisturizer, hair gel, hair spray, and thick sunscreen. People with milia eyelid problems or milia on their lips should take a look at the ingredients in the products that they apply to these areas.
Long-term exposure to the sun
Milia can also develop as a result of sun damage. As the skin ages, its outer layer thickens, and this can interfere with the skin’s ability to slough off dead cells. Thicker skin is also more difficult to successfully exfoliate.
Porphyria Cutanea Tarda
Milia are sometimes linked to skin diseases such as Porphyria Cutanea Tarda (PCT), a blistering disorder. The good news is that this condition is uncommon — there is certainly no reason to assume that you have a blistering disorder just because you have milia.
Even if you do develop PCT, other symptoms are likely to alert you to the problem. These can include blisters as well as new hairs on the face, knuckles, and the backs of hands.
Genetics
Some people simply inherit skin disorders or predispositions to certain issues.
What is the treatment for milia?
The first question to ask yourself is whether you even need milia treatment. “While milia are certainly an inconvenience, they are benign growths and don’t necessarily require treatment,” says New York City-based dermatologist Dr. Marina Peredo.
That said, there are plenty of people who do need milia removal, or who would simply prefer to have milia removed because they are bothersome or unsightly. According to Georgia-based dermatologist Dr. Alia S. Brown, there are many different treatments available for these people.
“Treatment ranges between over the counter exfoliants such as cleansers with granules in them to the new exfoliating brushes made by Clarisonic or Neutrogena,” says Brown. “When these modalities aren’t effective, patients will get success with extractions done under the care of a licensed aesthetician or dermatologist, as well as microdermabrasion.”
Not everyone needs an in-office treatment. Some cases can be treated with a milia home remedy.
Exfoliation
“Many milia can be treated by exfoliating which causes cell turnover thus gradually eradicating the milia,” says Dr. Stan Kovak, a cosmetic physician located in Oakbrook Terrace, IL.
Exfoliation keeps the outer layer of skin smooth and thin, and can be particularly effective for eye milia patients. However, only gentle exfoliant scrubs, as recommended by your dermatologist, should be used.
Retinol
Another potentially helpful remedy is retinol. These products should not be used on the eyelids unless a dermatologist has specifically instructed you to do so, says Sarasota, Florida-based dermatologist Dr. Jennifer Trent “Always be gentle when treating the eye area,” she cautions. “And always consult with a dermatologist before beginning a regimen.”
For other areas of the face, the application of a pea-sized drop of retinol every other night should suffice. Do so after cleansing.
In-Office Removal
In some cases milia won’t go away no matter what you do on your own. If this happens, you most likely need to pay a visit to your dermatologist to have the milia extracted. Typically, this entails cleansing the skin with an antiseptic, opening the skin above the milia with a sterile instrument, and then applying pressure with a milia removal tool called a comedone extractor.
As New York City-based dermatologist Dr. Suzanne Jennifer Friedler points out, “dermatologists may also use other techniques to remove milia such as electrodessication, chemical peels, or dermabrasion.” CO2 laser vaporization has also been used to effectively treat multiple types of milia.
Friedler says that incision and drainage is favored when there are only a few lesions, and other techniques are usually reserved for widespread areas and for patients with other problems that may benefit from the treatment, such as wrinkling or photo damage.
Treatment also depends on the area affected. For example, says Trent, “care has to be exercised when treating the delicate areas of the body, such as the eyelids.”
The upper eyelid is, in fact, one of the trickiest spots to remove milia from. Since a dermatologist can’t push on the area without harming the eyeball, the lid has to be pulled up or to the side, and this can be difficult.
Crack the mystery behind Milia removal
White bumps that appear on the skin are referred to as Milia. They are usually grouped and can appear anywhere in your body. We have curated a list of products that may help you.
BEZOX Professional Acne Removal Needle
High-quality steel, easier to point out the whiteheads, blackheads, comedones, acne, and pimples. Non-toxic silicone cap will protect the needle tip and avoid acupuncture and exposure of the needle tip. They are portable. The needle will not cause any skin allergies. They are designed with a practical and dual-end design.
Diva Stuff Milia Treatment Cream
Milia Treatment Cream with salicylic acid that has an exfoliating effect . It sweeps inside your follicle that helps loosen up a plug. With retinol liposomes, this cream also helps open up the Milia and prevents more from forming in the first place.
Best Skin Exfoliator for Acne Prone & Milia
Skin Exfoliator will help you remove the milia, blackhead, whitehead, splinter, pimple, zit, deep cystic acne, splinter, pus around your nose, forehead, cheeks, chin, and anywhere in your body. Skin Exfoliator is designed with good quality steel and is durable with a good grip, recommended by dermatologists.
BESTOPE – Blackhead Remover Pimple Popper Tool Kit
BESTOPE toolkit is the multifunctional set that removes milia. This toolkit works for all types of skins. The toolkit has an anti-slip handle that controls pressure. They are easy to use without any damage to the skin. Use alcohol and clean the tool before and after use.
Types of Milia
There are several types of milia, classified according to age or the type of injury or condition that causes them to develop.
Primary milia
Primary milia occurs when keratin is trapped under the surface of the skin. This type of milia usually occurs on the eyelids, forehead, or even the genitals, and may disappear on its own within a few weeks or months.
Secondary (traumatic) milia
Secondary milia are tiny cysts located in skin areas that have experienced an injury, burn or blistering. They often appear red around the edges and white in the middle.
Neonatal milia
Neonatal milia are perhaps the most common form of milia. Milia on newborns usually appears on the face, scalp, and torso.
Juvenile milia
Juvenile milia usually stems from genetic disorders such as pachyonychia congenital, Bazex-Dupré-Christol syndrome, nevoid basal cell carcinoma syndrome, or Gardner syndrome.
Multiple eruptive milia
Multiple eruptive milia is often characterized by itchiness. It typically occur on the face, arms, and torso. These bumps can last anywhere from weeks to months.
Drug-related milia
Though rare, milia can also develop as a result of steroid cream use.
Milia en plaque
This type of milia is often associated with autoimmune or genetic disorders, such as lichen planus or discoid lupus. Milia en plaque can be found on the ears, cheeks, jaw or eyelids. It most commonly affects middle-aged women, but can also affect all adult milia sufferers and children.
How do you prevent milia?
At this point, you’re probably still wondering what you can do to prevent milia from appearing in the first place. The experts we interviewed had lots of tips.
All of them stressed that thick creams and makeups should be avoided if you’re looking to prevent milia. They also agreed on the importance of keeping your face clean. Consider using a buffered glycolic acid to get rid of surface debris and clean your pores.
It is important to exfoliate a couple times a week, if possible.
Also, don’t forget to protect yourself from the sun. “Sun damage is a known contributor to milia formation, so ensuring you have a good sunscreen incorporated into your daily routine is key,” says Peredo.
Trent emphasizes that it is important that you avoid picking at milia, because you could end up with a scar.
Friedler stresses that one milium doesn’t mean that you need to rush to the dermatologist. However, if you have many — or particularly long-lasting — milia, it’s probably time to make an appointment.