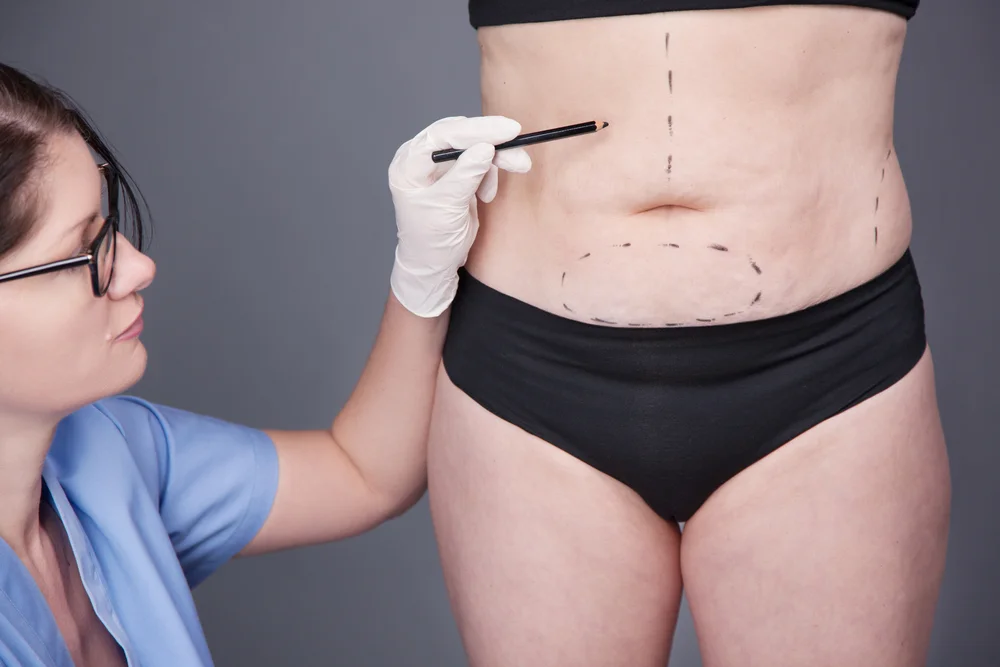
- A panniculectomy is a common surgical procedure performed to remove significant excess hanging abdominal skin after major weight loss.
- It is a safe and effective procedure when performed by a skilled plastic surgeon, but is not without risks and complications
- It is important to follow the surgeon’s postoperative regimen and instructions to maximize the chances of optimal outcome
What is a panniculectomy?
A panniculectomy is the name of the surgical procedure that removes a pannus, which is an apron of excess abdominal skin that hangs over the thighs and genitals, usually as the result of rapid massive weight loss.
A pannus will frequently cause back pain and skin rashes in the pubic area.
Panniculectomy procedures are often necessary not only to improve personal hygiene and mobility. As Boston based plastic surgeon Dr. Samuel Lin points out, “a panniculectomy helps patients with the rashes and irritation that occur under the pannus of the abdomen”.
A panniculectomy will also leave patients with a slimmer appearance, helping them look better both in and out of their clothes, and by extension doing a world of good for their self-confidence.
Panniculectomy candidates
Panniculectomy patients are most commonly individuals who were once critically overweight but have since shed many pounds, often following a gastric bypass or other bariatric surgery procedures.
Losing a significant amount of weight this way typically leaves a large amount of excess skin behind.
Ideal candidates for this procedure:
- Are bothered by excess skin below the lower abdomen following dramatic weight loss or pregnancy
- Are physically healthy and at a stable weight
- Are non-smokers
- Have realistic expectations of the procedure’s outcome
As postpartum women also comprise a significant portion of the candidate pool for the operation, it’s not uncommon for it to be performed in conjunction with mommy makeover procedures.
Panniculectomy vs. abdominoplasty
While panniculectomy surgery is often confused with abdominoplasty (tummy tuck), these two plastic surgery procedures are different.
- A panniculectomy ONLY removes excess skin and tissue from the lower abdomen under the belly button
- An abdominoplasty removes excess skin and tissue from the lower abdomen under the belly button AND tightens the abdominal muscles.
According to Salt Lake City based plastic surgeon Dr. Renato Saltz, “a panniculectomy addresses the excess skin and fat layers only, without repairing any muscle separation. If the patient has a rectus diastasis, where the two rectus abdominis muscles are separated at midline, commonly seen after pregnancy or any other large abdominal mass or hernia, a plication (suturing the muscles together) will be necessary. This procedure is called an abdominoplasty.”
Panniculectomy procedure
The procedure should be performed by a qualified plastic surgeon.
The procedure typically takes between two and five hours from start to finish, depending on the patient, the surgeon, and if other procedures are performed simultaneously.
As Dr. Samuel Lin explains: “Panniculectomy by itself is a procedure that takes me two to three hours to complete, but when combined with other procedures can take between three and six hours in total.”
The incision for a panniculectomy is very low along the bikini line, usually in the crease where the pannus is folding over the pubic area. It extends from hip to hip and may extend beyond that if the pannus extends to the sides. In some cases, if the pannus extends around the back, the incision may go all the way around the body. In such cases, the procedure is called a circumferential or “belt” lipectomy (as the incision looks like a pants belt).
In cases where the patient has a lower abdominal pannus with significant excess skin and fat on the flanks/sides, an “anchor incision” may be used with a vertical component that extends from the pubic area up the middle of the abdomen to just below the chest. This is called a “fleur-di-lis” procedure and is very effective at reducing both the vertical skin excess at the lower abdominal pannus and the horizontal skin excess at the flanks.
Any excess fat is removed and the skin is contoured and sutured into the new configuration.
The navel (belly button) generally gets repositioned during procedure.
- A large panniculectomy may result in the loss of the navel, with some doctors even charging an additional fee just to save your belly button.
- Your doctor should express the likelihood of this possibility over the course of your initial consultation. If not, ask them what their policy is so far as preserving navel’s is concerned, especially if keeping it results in additional fees.
Panniculectomy before & after pictures
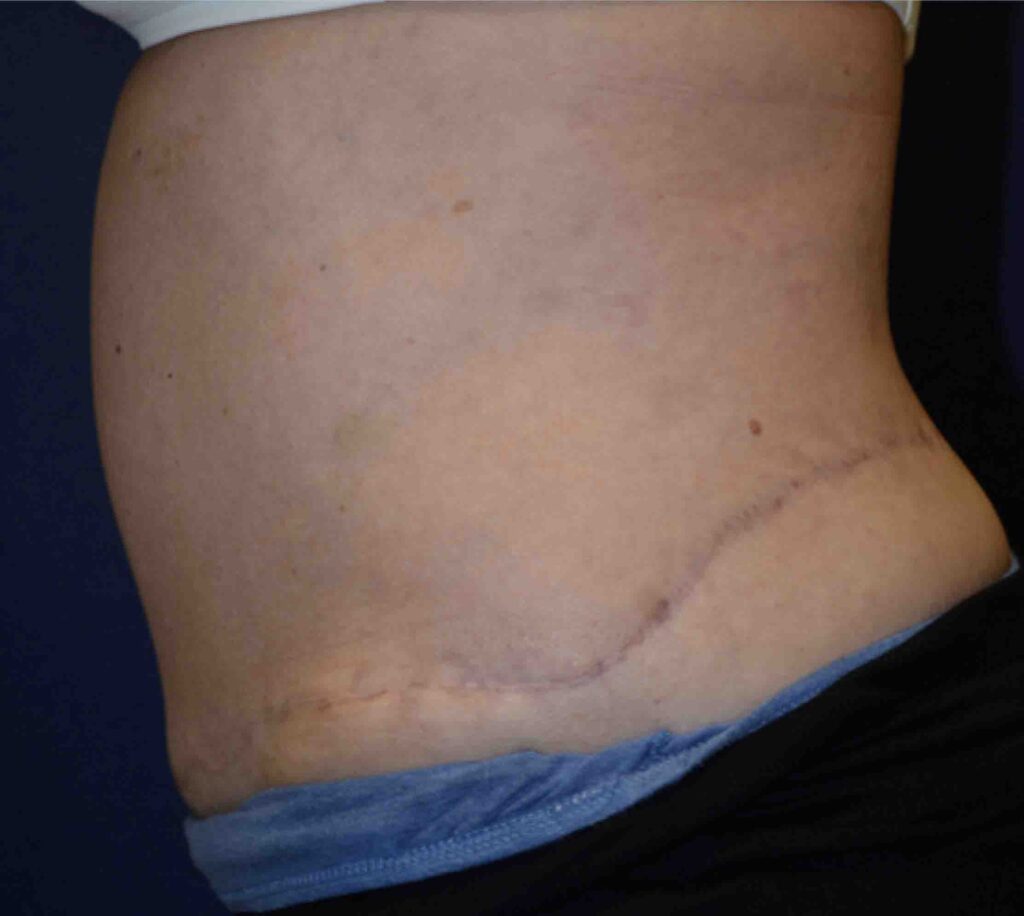
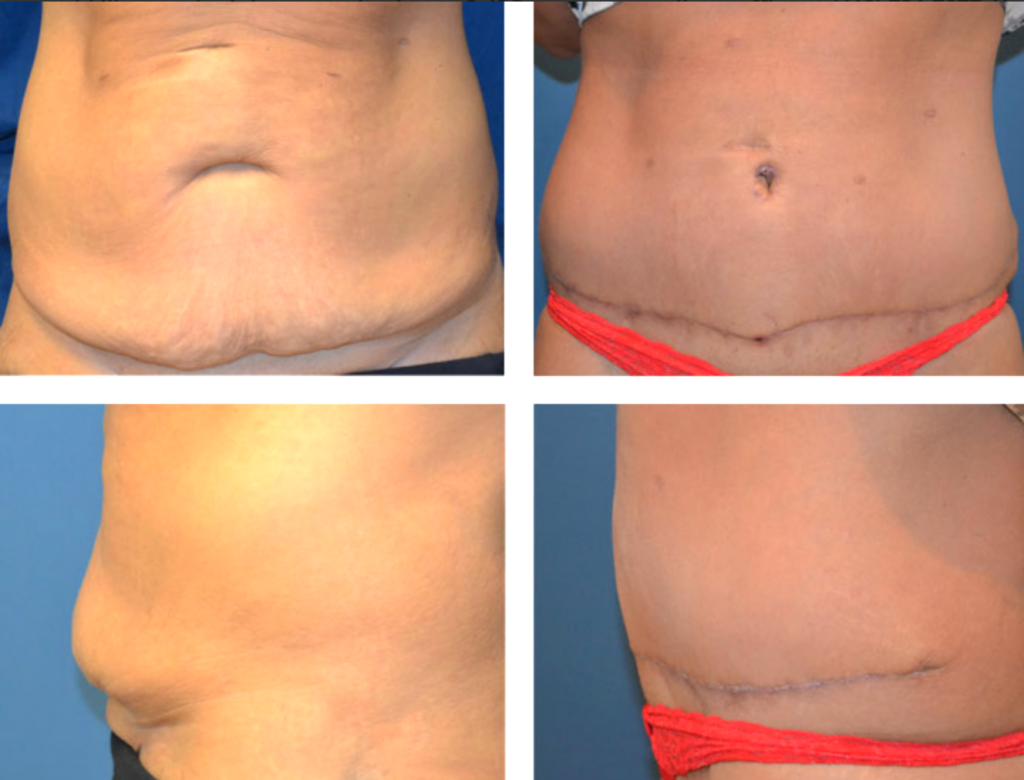
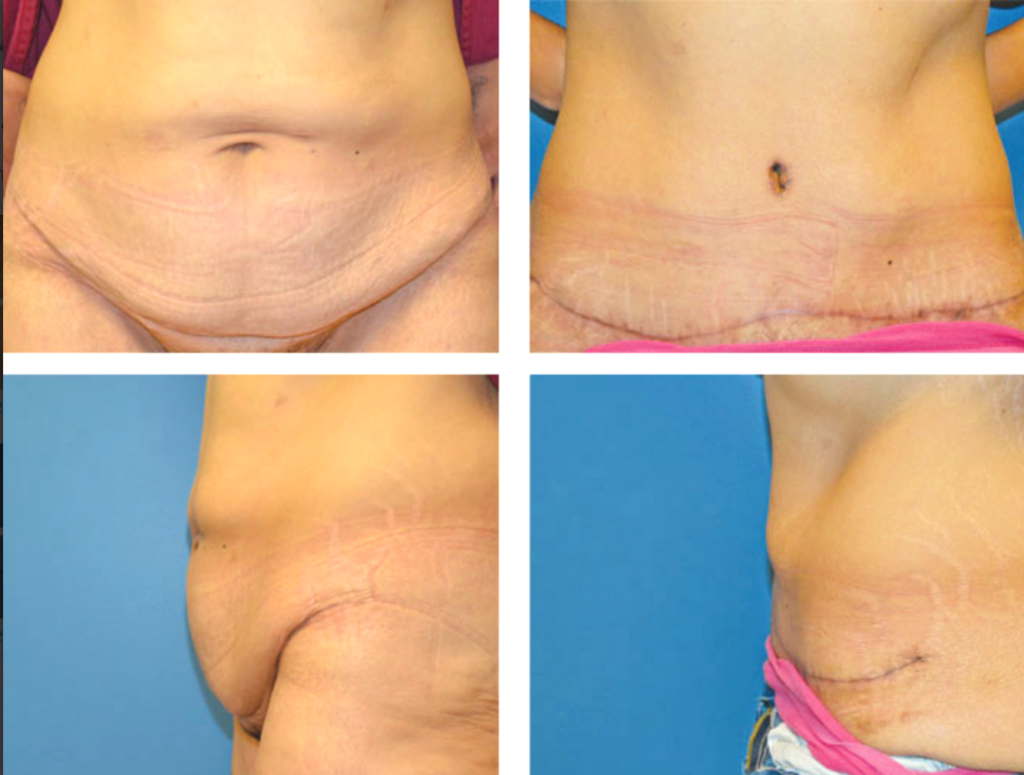
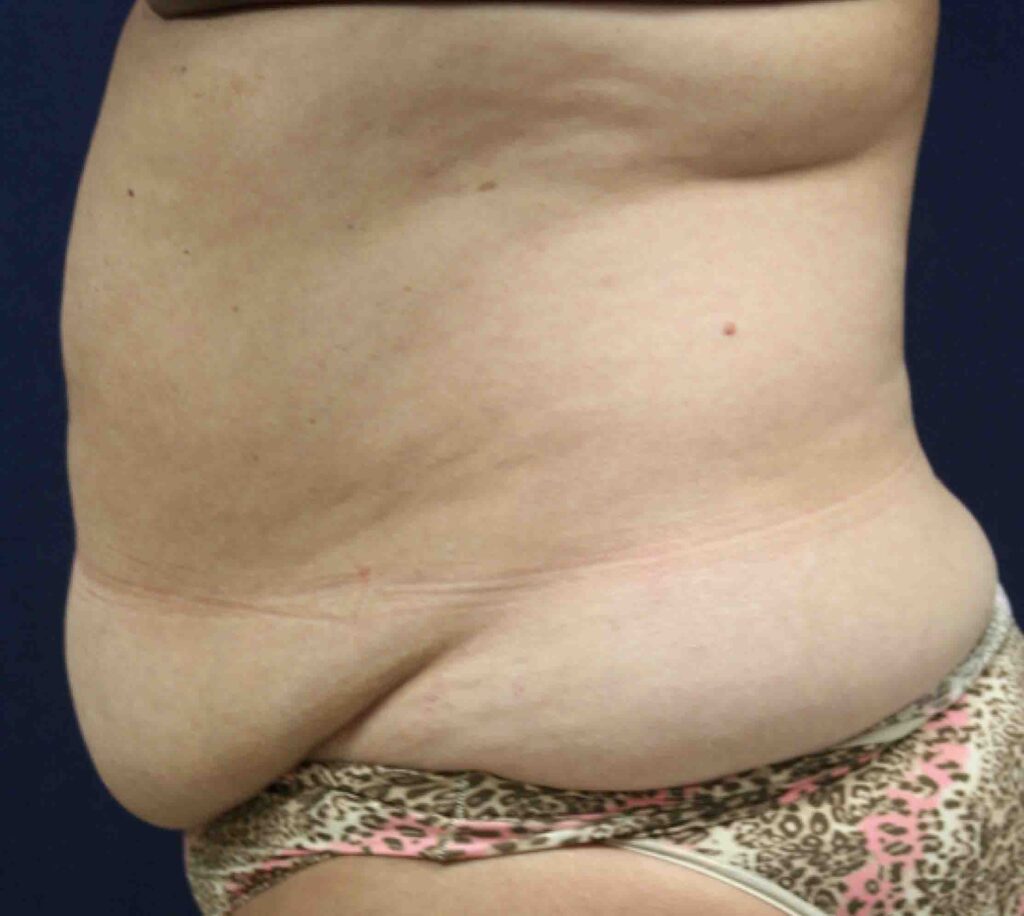
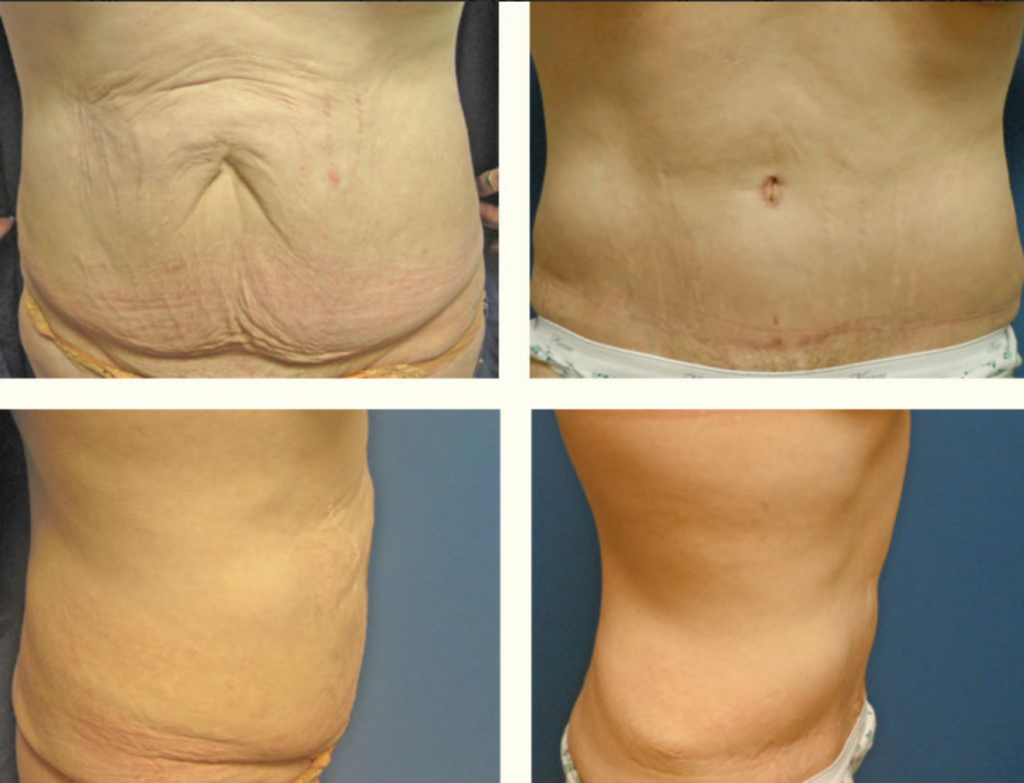
Panniculectomy recovery
For small to moderate panniculectomy procedures, patients may be able to go home the day of the surgery. In larger cases, patients may remain in the hospital anywhere from one night to a few days postoperatively.
Over this period drains are usually inserted into the patient’s incisions in order to extract any excess fluids, and later removed once the levels of fluid extracted are consistently low over a given period of time determined by the physician.
Initially, sponge baths will be the only bathing permitted. Patients are usually permitted to shower after 2 days.
Compression garments will most likely be prescribed so that the belly area is consistently supported while healing.
Patients can expect the relatively moderate levels of pain, bruising, and swelling in the immediate 3-7 days postoperatively.
Pain is well controlled with narcotic medications, and may be dramatically reduced with Exparel liposomal bupivacaine injected by the surgeon at the time of the procedure.
Bruising and swelling diminish significantly over 6-12 weeks. This can be expedited with healing supplements such as arnica and bromelain, and modalities such as LED light therapy and lymphatic massage.
Light exercise can begin after 10-14 days. Any demanding exercise, heavy lifting, or sporting activities will be off limits for at least six weeks following the operation.
Scar regimens to reduce the appearance of scarring and may include scar creams, gels, and silicone sheeting, are generally begun at 4-6 weeks postoperatively after any scabs have fallen off.
Full recovery can take several months for some people, and as with any medical procedure it’s important patients pay strict attention to all of the post-operative instructions provided to them.
As Paramus, NJ based plastic surgeon Dr. Frank Ferraro points out, “recovery from a panniculectomy is very similar to recovering from an abdominoplasty, which is to say, like the procedure itself, not particularly risky.”
Panniculectomy scar
Panniculectomy risks and complications
Potential complications and side effects include:
- Infection
- Wound separation/breakdown
- Excess fluid in the abdomen (seroma)
- Bleeding (hematoma)
- Skin necrosis/loss
- Skin discoloration
- Numbness
- Excessive scarring
- Fat necrosis/hardening of tissue
- Residual/recurrent loose skin
- Asymmetry
- Neuroma/nerve pain
- Blood clots
- Poor cosmetic result
- Need for revision surgery
Cost
The cost of a panniculectomy can, and will, vary depending on a wide array of factors:
- the extent of the procedure
- the volume of skin removed
- the city where the patient is being treated
- the experience and reputation of the practitioner performing the operation.
The average patient can expect to pay between $7,000 and $12,000 for this procedure when performed in the United States.
In some cases health insurers will pick up the tab as there are basic, arguably essential, health benefits to be derived from this surgery.
If it is determined that the patient’s condition inhibits “daily activities of living,” treatment required to eliminate or reduce such interference may be covered.
Purely cosmetic procedures are never reimbursed by medical insurance.
Alternative options
Before electing to have a panniculectomy, patients should speak to their provider to see if there are other realistic alternative treatments to consider.
While the majority of people who need a pannus removed from their abdomens will require surgery, in some instances it may be possible to achieve acceptable results through a combination of liposuction and various other treatments.
That said, it’s totally unrealistic to expect liposuction alone to remove an amount of tissue as large as a pannus and somehow miraculously leave patients with tighter skin and a nicely contoured belly immediately afterward.
Nevertheless, patients should discuss all potential options with their doctors to see which holds the most promise for them personally and determine whether a panniculectomy, perhaps combined with another procedure, will indeed lead them to the best possible conclusion.