- You don’t have to be using topical steroids to develop topical steroid withdrawal.
- Symptoms of red skin syndrome can extend to more than just your skin.
- There is no cure for red skin syndrome, but there are ways to manage symptoms.
- It can take years for red skin syndrome to clear up.
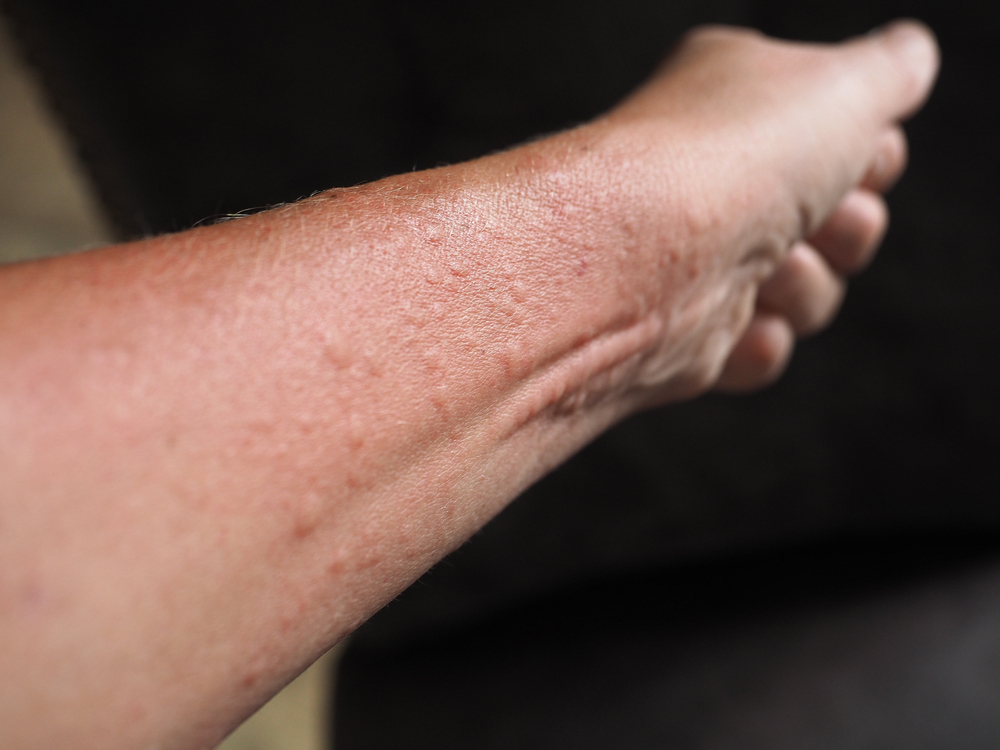
Red skin syndrome (RSS) is a bright red rash, often accompanied by the itching and burning associated with topical steroid use.
The aptly named condition can sometimes look like a widespread burn or severe eczema. However, it’s important to identify RSS for what it is. If misdiagnosed and treated with the same topical steroids that precipitated the condition, then it could get much worse.
What causes red skin syndrome?
RSS can result from the long-term use of topical steroids. For this reason, it’s also sometimes referred to as topical steroid addiction (TSA) or topical steroid withdrawal (TSW).
This connection to topical steroids makes RSS extremely difficult to diagnose. After all, if you’re taking a topical steroid, then you’re already treating a skin condition, many of which have similar symptoms to RSS.
RSS can occur while you’re still taking the steroid. When this happens, you may notice that the steroid is less effective in treating your symptoms, resulting in a mixture of RSS symptoms and the worsening of symptoms for your existing skin condition.
In some cases, RSS may present itself within days or weeks of stopping the steroid. This may be easier to detect, but could still be mistaken for a flare-up of the original skin condition.
Who is at risk for red skin syndrome?
People who are currently taking or recently stopped taking topical steroids for skin conditions, such as acne, eczema, and dermatitis, are at risk. However, any regular contact with steroids could present a problem.
For example, if you are a caregiver applying topical steroids to someone else, you could still develop the condition. That’s why it is so important to wear gloves or wash your hands immediately after administering a dose.
According to the National Eczema Association, women, particularly those who blush easily, are at greater risk of developing RSS. They also note that the use of steroids on sensitive parts of the body, like the face or genitals, presents a greater risk of developing RSS.
Finally, people who are using more than their recommended dose of topical steroids, or for longer than prescribed, are at the greatest risk of developing RSS.
How common is red skin syndrome?
RSS has not been extensively studied. At present, there are no statistics showing how common RSS is in general. However, a 2003 Japanese study showed that 12% of adults who were using topical steroids to treat dermatitis developed RSS.
What are the symptoms of red skin syndrome?
This depends on whether you’re still using the steroid in question and what exactly you mean by Red Skin Syndrome.
If you are still using the steroid, you’ll notice that it’s becoming less effective against your skin condition, leading to flare-ups of the existing condition. Additionally, you may notice the following:
- Redness even in areas where the steroid isn’t being applied.
- Increased itching, burning, or stinging.
- A dry flaky rash (similar to eczema).
If you’re no longer taking the steroid, your symptoms will likely be more severe. As your body goes through topical steroid withdrawal, symptoms tend to fall into one of two categories.
- Erythematous-Edematous — This is characterized by red, sensitive skin that worsens at the site of the original rash and spreads beyond it. It may include blistering and swelling from fluid build-up. It may also include crinkly and dry skin that breaks easily.
- Papulopustular — This is characterized by small bumps. It often occurs in the face, a condition called steroid rosacea, regardless of where the steroid was applied. It can also come with redness, swelling, and irritation.
Sometimes papulopustular rashes are considered a type of RSS, while others use RSS to refer exclusively to erythematous-edematous type rashes, sometimes just calling them “red burning skin.”
RSS doesn’t just affect the skin. Regardless of the form your topical steroid withdrawal takes, you may experience the following after stopping the medication.
- Changes in appetite, including weight gain or loss.
- Changes in sleep patterns, often accompanied by fatigue.
- Dry, sore eyes.
- Hair loss or thinning.
- Nerve pain.
RSS sufferers have also reported depression and anxiety as they struggle to manage their condition.
» If you are experiencing these symptoms, meet our Medical Review Team and get an opinion before jumping into any conclusion.
How is red skin syndrome diagnosed?
RSS that stays close to the location of the original skin condition can be difficult to diagnose, especially if the symptoms are similar. However, RSS frequently spreads to other parts of the body, even places that did not come into contact with the topical steroid.
If you’re taking or have recently stopped taking topical steroids, your physician may instinctively suspect RSS. Nevertheless, he or she will first likely perform a patch test to rule out other possibilities. Some physicians might also attempt a skin biopsy, but its efficacy in determining RSS has been called into question.
How is red skin syndrome treated?
If you’re still using topical steroids, you’ll need to stop. Do so under the guidance of your physician. Some doctors may have you taper off the the drug slowly, while others may want you to stop immediately.
This won’t cure you of the condition and, in fact, you can expect your symptoms to worsen at first while your body goes through sudden topical steroid withdrawal. It’s nevertheless essential to stop using the steroid in order to eventually improve.
There is no simple cure for RSS, but there are ways to manage the symptoms. Your doctor may prescribe any one or a combination of the following:
- Painkillers — Treats the burning and stinging.
- Antihistamines or other immunosuppressants — Helps with itchiness and swelling.
- Antibacterial ointment or antibiotics — Helps prevent infection of sensitive skin.
- Sleep aids — Helps you to rest, treating fatigue and depression.
Certain painkillers and antihistamines can be purchased over-the-counter as well. However, you’ll need to consult with your dermatologist before taking any over-the-counter treatments for your condition.
Finally, in some cases, oral steroids have been used to treat existing and new skin symptoms, as it appears the addiction only applies to topical steroids. However, the medical community remains mixed on this and most other treatments.
The good news is that with symptom management and the cessation of topical steroids, your condition should resolve itself with time.
» Curious about these or other RSS treatments? Meet our Medical Review Team.
How is red skin syndrome prevented?
Despite the obvious downsides to topical steroid use, it’s sometimes necessary to take them to effectively treat of a host of skin conditions. There’s no guarantee you won’t suffer any ill-effects from topical steroid use, but if you take certain precautions you can significantly better your odds.
Wash your hands after administering topical steroids to yourself or others. If your hands are part of the treated area, avoid rubbing the steroid on other parts of your body.
Use the topical steroid only as prescribed. This means no applying excess amounts of the steroid in one sitting, no applying it more frequently throughout the day, and no using it for longer than the prescription allows.
Should you notice any new or worsening symptoms developing while taking the steroid, contact your prescribing physician immediately.
Are there home remedies for red skin syndrome?
There is no at-home cure for the condition. However, there are things you can do to alleviate symptoms.
- Cold compress — Helps alleviate itch and burning pain.
- Vaseline — Keeps your skin moist, protecting against flaking and breaking.
- Epsom salt and oatmeal baths — Soothes itchy burning skin.
- Special soaps and detergents — Prevents further irritation to sensitive skin.
- 100% cotton clothing — Softer materials are easier on sensitive skin.
- Nutritional supplements — Healthy skin heals faster.
While there’s no guarantee these methods will help you, they could be worth a try, and your dermatologist may even recommend them.
How long does recovery from red skin syndrome take?
It can take anywhere from weeks to years to recover from RSS. How long it takes you personally to recover will depend on a variety of factors, including the strength of the steroid you used, the length of time you used it for, and the extent of your RSS.