- The term “sebaceous cyst” is applied to a number of different types of cysts, causing some confusion.
- Sebaceous cysts are not cancerous, but cancerous growths can sometimes be mistaken for cysts.
- If not completely removed, sebaceous cysts can return repeatedly.
Laymen and medical professionals alike often erroneously use the term “sebaceous cyst” to refer to a range of cysts with similar qualities. Here’s what you need to know about these fairly common skin growths — before taking matters into your own hands.
What is a Sebaceous Cyst?
In most cases “sebaceous cyst” refers to an epidermoid cyst, which grows from the surface of the skin (epidermis). It can less commonly refer to a pilar cyst, which grows from a hair follicle.
Often, these two terms are used interchangeably. However, a true sebaceous cyst, which grows from the sebaceous gland, is extremely rare and most commonly associated with a genetic condition called steatocystoma multiplex.
If you have this condition, you’re probably already aware. It occurs at puberty and produces several of these cysts at once. Still, for reasons not yet completely understood, it is also possible to get a single sebaceous cyst, which is called steatocystoma simplex.
Epidermoid cysts, pilar cysts, and independently forming true sebaceous cysts (steatocystoma simplex) are all functionally the same when it comes to matters of treatment and removal. Here they’ll all be referred to collectively as sebaceous cysts.
Understanding Cysts
Your skin, hair, and finger- and toenails are continuously replacing themselves. Skin cells multiply at an incredible rate in order to replace old cells, which are then shed from your body. In fact, your skin is completely replaced every 27 days. If some of those regenerating cells get trapped, a sac forms from them, collecting even more cells inside itself, sometimes alongside gas, fluid, blood, or pus.
This is the description of an epidermoid cyst. These cysts contain a variety of elements, most notably keratin, the same substance that makes up hair, nails, and the outer layer of the skin. Pilar cysts too are filled with keratin, whereas true sebaceous cysts are filled with sebum, the oily substance that’s normally secreted from the sebaceous gland onto the surface of the skin as a lubricant.
Despite these distinctions, all three types of cysts are formed when cells fail to function normally and trap important substances in a sac under the skin instead of releasing those substances onto the skin’s surface.
Causes and Symptoms
How exactly does this happen? There are numerous possible causes. It may never be completely clear what caused a cyst. Fortunately, in most cases it doesn’t matter.
- Trauma — Damage to an area can lead to blockages, which in turn lead to cysts. The inciting trauma, which can include scratches or burns, sometimes happens months before a cyst finally develops. Damage can also occur to glands, hair follicles, and the skin during surgery.
- Skin condition — Acne in particular is known to cause these types of cysts. As with trauma, acne can cause blockages or otherwise interfere with the normal functioning of glands and hair follicles.
- Swollen hair follicle — Hair follicles swell when they become infected or inflamed, as from folliculitis. This too can lead to blockages.
- Deformed duct — Sometimes the follicular ducts that connect sebaceous glands to hair follicles are deformed or misshapen, either at birth or from later trauma. These deformities may interfere with the secretion of oils from the sebaceous gland.
- Genetic condition — While it’s not possible to directly inherit a cyst, it is possible to inherit conditions that can lead to cysts. Gardner’s syndrome leads to epidermoid cysts as well as other growths. Basal cell nevus syndrome, which results in cancer (basal cell carcinoma) just after puberty, can also cause these types of cysts.
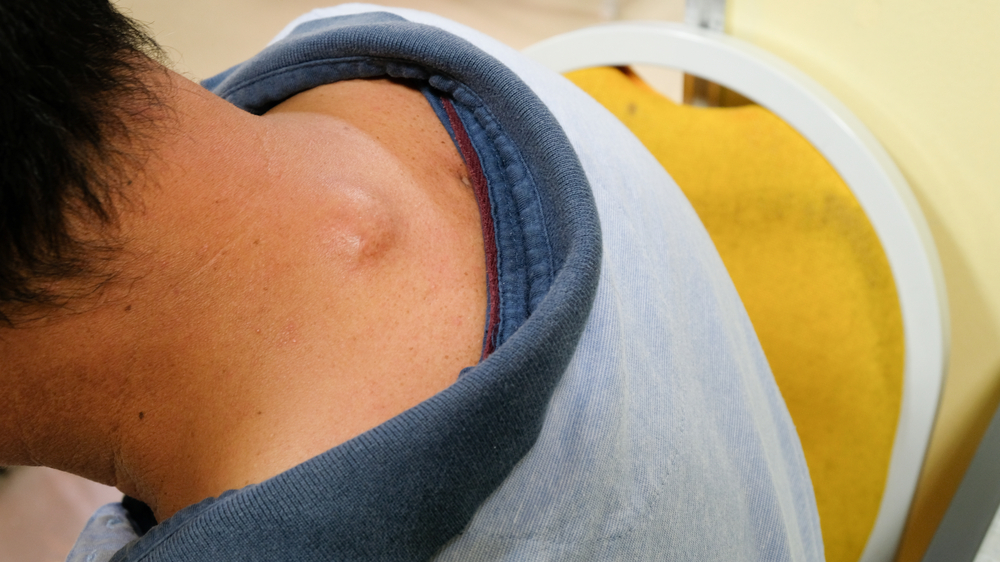
Whatever the cause, you’ll likely experience very little if any discomfort. A cyst may feel firm or soft depending on what type of cyst it is. Regardless, sebaceous cysts in all their forms are usually small, slow growing, and benign.
Other symptoms may accompany a cyst, like a small, crusted spot on the top of the cyst, as with epidermoid cysts, or a warming of the skin near the cyst. Although there may be minor physical differences between the different types of cysts, those differences are inconsequential.
If left untreated, sebaceous cysts could get larger. Large cysts may be tender, uncomfortable, or even painful. Often whether a cyst is more or less tender depends on where it’s located on the skin and whether or not it regularly comes into contact with clothes or other skin.
» If you suspect you have a sebaceous cyst, meet your physician immediately and get examined of your cyst.
Complications and Cancer
When it comes to sebaceous cysts, the primary complication is infection. Infected cysts are significantly more painful, and untreated infections can spread. If you notice redness or warmth around the cyst, or if there’s a pus-like (purulent) discharge, then the cyst is likely infected.
When a cyst becomes infected, it’s typically due to a burst or tear in the cyst itself. This can happen when the cyst repeatedly rubs against skin or clothing. It can also happen if the cyst is repeatedly touched or intentionally punctured to release the fluid inside.
Sometimes, a cyst is not really what it seems. Although sebaceous cysts are not cancerous, cancerous cysts or growths can be easily mistaken for this harmless condition. Growths should always be examined by a medical professional in order to rule out the possibility of cancer.
While it’s almost always a good idea to talk to a doctor, there are certain signs in particular that can indicate your cyst may really be a cancerous growth. If the cyst is larger than 5mm in diameter or grows quickly, it could be cancerous. The same is true for any cyst that returns quickly after being removed.
If a doctor has determined that your cyst is not cancerous, then it is not life-threatening. In fact, in many cases there may not even be a need to not have it removed at all. Still, cysts that go untreated will likely grow and may become more unsightly or uncomfortable.
The Dangers of Home Removal
As with zits or blisters, some people want to get rid of unsightly growths as quickly as possible, even if that means doing it themselves. It’s tempting to just pinch or pull a cyst until it bursts. As easy as this may sound, you absolutely should rely on a medical professional to remove your cyst.
Bursting a cyst yourself is ultimately not going to be successful. Even if the fluid drains, the sac will remain, leaving the very likely possibility that the cyst will reform. In all likelihood, that burst cyst will lead to an infection as well.
It’s eve riskier to attempt to excise your own cyst, sac and all. This requires surgical precision. Without it you could seriously damage your skin and the surrounding tissue, and the risk of infection is even greater.
If you are intent on having your cyst removed, see a dermatologist and have it done properly. In the meantime, keep your cyst clean and protect it from irritation.
Medical Treatment for Sebaceous Cysts
A dermatologist will be able to diagnose a cyst in order to determine whether or not it’s cancerous. This generally involves a physical examination of the cyst and a review of your medical history. In some cases, the dermatologist will examine the cyst with an ultrasound.
If the dermatologist suspects cancer, he or she will perform a punch biopsy, wherein a small portion of the growth is removed and sent to a pathologist for examination. If the growth is not cancerous and is in fact a sebaceous cyst, there are three options: leave the cyst alone, drain the cyst, or remove it completely.
It may be perfectly fine just to let your cyst be. Surgery can come with complications, like infection and scarring. If a cyst is small and in an inconspicuous place, having it removed may not be worth the effort. In some cases, sebaceous cysts may even go away on their own.
If your cyst is small but in a location where it’s likely to get irritated by rubbing against clothes or skin, your dermatologist might recommend drainage. Drainage can be done manually or with the help of a carbon dioxide (CO2) laser. This removes the contents of the cyst, but leaves the cyst sac. As already mentioned, the presence of a sac makes it more likely that the cyst will grow back, but it’s also possible that it won’t.
The third option is complete removal. Your dermatologist (or surgeon) will remove the cyst, sac and all. This is more common in the case of large cysts that have become uncomfortable or painful due to their size. Large cysts are also less likely to go away on their own and more likely to regrow if drained. Removal can be done in several different ways, but in all cases the result is similar.
- Surgical excision — Your dermatologist numbs the area and uses a scalpel to cut away the entire cyst sac.
- Cryosurgery — The cyst is frozen using liquid nitrogen, killing the tissue, which falls away.
- Electrosurgery — High-frequency radio waves heat and kill the cyst tissue.
- Laser-assisted removal — A CO2 laser is used to drain the cyst. About a month later, when the cyst wall as shrunk, the whole structure is removed.
Prior to performing any of these procedures, your dermatologist will likely do a CT scan to get a better look at the cyst and determine the best method for removal.
When to See a Doctor
You may be apprehensive about seeking medical attention for that small growth on your skin. While it’s recommended that you consult a dermatologist about any and all mysterious growths, not everyone can afford to see a doctor about every abnormality on their skin.
If you decide to wait, be wary of cysts that are abnormally large, grow rapidly, or become infected, which can be signaled by redness, pain, or inflammation. You should also see a doctor if the cyst is recurring or uncomfortable.
Lastly, there’s nothing wrong with seeking a surgical solution for cosmetic reasons. Cysts in visible places, like the face, can be emotionally difficult to tolerate. You dermatologist can help.
» If you’re ready to talk to a dermatologist about your sebaceous cyst, meet our medical review team.