- Seromas are fluid collections that can appear under the skin following a surgical procedure.
- It is important to recognize the early signs and to alert your doctor to help to prevent more serious issues like a secondary infection.
- A seroma, which is generally considered benign, is not to be confused with a hematoma which in some cases can be life-threatening.
What is a seroma?
A seroma is a collection of fluid that develops under the surface of the skin following a surgical procedure.
Also known as serum or serous fluid, this clear discharge of fluid is triggered by the injury and subsequent death of cells, typically along an incision or where skin tissue was removed.
In some cases, seromas will cause the tissue surrounding the area to harden over time, creating a knot of calcified scar-like tissue. This knot can remain even after the serous fluid has been absorbed by the body.
What causes a seroma?
When blood vessels and lymphatics get damaged through the normal course of invasive surgical procedures, the body mounts an inflammatory response, resulting in the production of clear fluid.
The body is able to absorb a certain amount of this inflammatory fluid each day. When the fluid is produced at a greater rate than the body is able to absorbing, the fluid can collect in the area where the surgery was performed, resulting in a seroma.
Where do seromas form?
While seromas can occur after even minor surgery, they are most common following more extensive plastic surgery procedures, including:
- Abdominoplasty (Tummy tuck)
- Hernia repair
- Breast reconstruction (following mastectomy for breast cancer)
- Breast augmentation
- Liposuction
Tummy tuck seromas
Seroma is the most common complication following a tummy tuck, but most doctors do not consider it a serious condition. Seromas can also occur following hernia repair, a procedure that is often performed during diastasis recti surgery.
According to the NCBI, up to 38% of patients who get an abdominal procedure (tummy tuck, panniculectomy, or transverse recti surgery) will experience a seroma.
It is important to note that patients who suffer from obesity are more likely to experience seroma following a tummy tuck. This is one reason why doctors often advise patients to lose weight before the procedure.
What are the symptoms of a seroma?
Some of the most common symptoms of a seroma include:
- Swelling
- Inflammation
- Tenderness
- Bruising
Seroma treatment
Not all seromas require treatment. For small seromas, the body will naturally reabsorb the fluid over time.
Larger seromas generally need to be treated to reduce the fluid contained in the seroma cavity and prevent new fluid from collecting. Note that seromas should only be treated by experienced physicians and should not be attempted by the patient.
In some cases where the seroma cavity does not appear to be superficial, an ultrasound or CT scan may be performed in order to determine the depth and volume of the fluid.
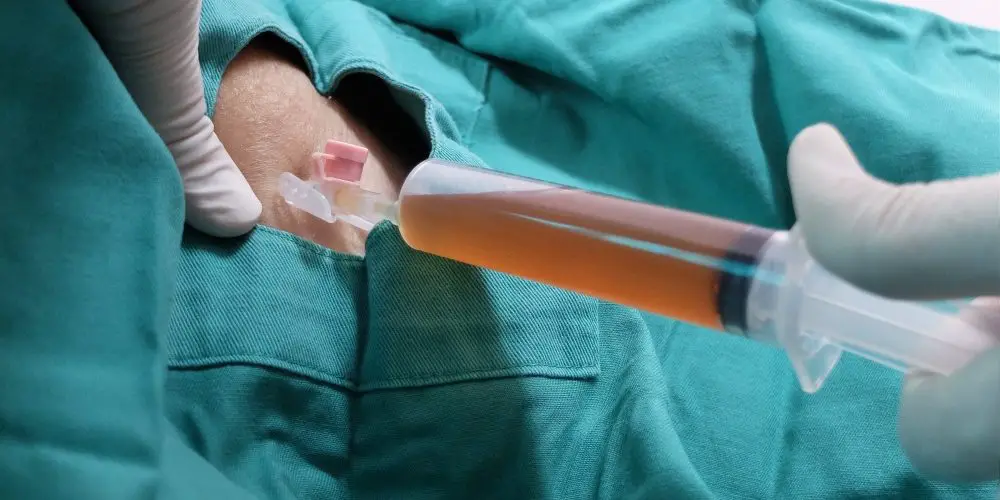
- Needle puncture aspiration
The doctor removes the seroma fluid by placing a hypodermic needle into the seroma cavity and aspirating the fluid with a syringe. This is the first line treatment option to drain a seroma, and may require multiple aspirations over the course of days to weeks as the seroma may recur.
- Drain Placement
For seromas that continue to recur following multiple aspiration attempts, a drain can be placed through the skin into the seroma cavity. The drain is then connected to a portable suction device, usually a suction bulb that is squeezed to collect the fluid. The drain is left in on constant suction until there is very little drainage coming from the seroma cavity over time.
- Injections
For stubborn seromas that continue to recur after multiple aspiration attempts and suction drain placement, certain substances, such as talc and antibiotics (tetracycline and doxycycline), may be injected into the seroma cavity, either following needle aspiration, or through a drain if present, to help prevent recurrence of the seroma. Injecting these substances irritates the lining of the seroma cavity, thereby causing inflammation. This inflammation triggers scar tissue formation, which can help obliterate the seroma cavity.
- Surgical removal
Chronic seromas that persist over the course of weeks and months and do not resolve despite regular draining and other treatments may require surgical intervention. The surgery entails exploring the seroma cavity, removing any scar tissue that may be present, suturing the tissues together to obliterate the cavity, and closing over a new drain.
Seroma infection and risk factors
In general, seromas are not considered life-threatening or dangerous. However, they can lead to several other complications when not properly treated.
The size of the seroma typically determines how serious the issue is. Larger seromas are more likely to trigger a secondary infection at the site.
Infection caused by a postoperative seroma is called a surgical site seroma infection (SSI). Your risk factor is higher if you are obese or have a compromised immune system or another condition that may delay or prevent your body’s ability to properly manage the infection.
If you have had a history of seromas following surgical procedures, make sure that your doctor knows so they can take extra precautions during recovery.
When to visit a doctor
If you are experiencing symptoms of seroma for several days following the removal of surgical drains, be sure to contact your doctor immediately so that they can treat the seroma and prevent infection.
Seek immediate medical attention if you experience any of the following symptoms:
- Fever
- Abnormal pulse rate
- An increase in pain, swelling, redness, and/or tenderness around the seroma
- Pus or bloody drainage from the seroma or incision site
How can seromas be prevented?
To prevent a seroma, surgeons will often install drainage tubes within the surgical treatment site in order to reduce fluid buildup during the healing process.
Unfortunately, seromas typically form after the drains have been removed.
During some surgical procedures such as abdominoplasty, surgeons may suture the overlying tissues down to the underlying tissues to help prevent a seroma.
Surgeons often also recommend the use of compression garments to minimize the risk of a seroma.
Seroma vs hematoma?
A seroma, which is generally considered benign, is not to be confused with a hematoma which in some cases can be life-threatening.
Whereas a seroma is made up of clear inflammatory and lymphatic fluid that is contained within a surgical cavity generally following an invasive procedure, a hematoma is made up of a collection of blood that results from damaged or leaking blood vessels caused by surgery, trauma, or other conditions such as a ruptured aneurysm, excessive anticoagulation medication, or a platelet deficiency.
Seromas tend to develop slowly over the course of days and weeks, exerting little pressure to the surrounding tissues. Hematomas tend to form more quickly over the course of minutes to hours, and may expand as a result of the involved blood vessels continuing to leak blood into the surrounding tissues. This is especially when due to arterial injury. Such expanding hematomas may be a surgical emergency and require immediate attention.
Left alone, stable, non-expanding hematomas will organize into clots, making them firmer than seromas which tend to be soft and compressible. While this makes hematomas resistant to standard drainage methods used to treat seromas, over time hematomas are generally absorbed by the body and do not require any intervention.
Post-Surgical Compression Garments: Top Products
Compression garments are needed during the recovery period of many invasive cosmetic surgery procedures. These tight socks, surgical bras, sleeves, and other specialized garments help to reduce swelling, promote proper healing, and prevent seromas. The compression garment that you choose should reflect your doctor’s recommendations and target the area of your procedure. Be sure to check sizing charts to find the right fit for the new you.

Camellias Womens Post-Surgery Front Closure Sports Bra
Camellias’ post-surgical bra provides comfort and support following breast related procedures like breast augmentation and breast reduction. The front clasps allow for ease of use during recovery when your mobility may be reduced. This garment is also infused with vitamin E for a natural healing boost.

Diane & Geordi Liposuction Compression Garments
Available in beige and black, Diane & Geori’s covers a large part of the body, making it perfect for post-liposuction wear. By conforming to natural curves, this garment can be worn seamlessly under most clothes. The garment also combines both hooks and zippers to provide a comfortable fit.

Larrycard Post-Arm Lift Compression Garment
Larrycard’s compression arm sleeves are perfect for post-liposuction and arm lift recovery. Available in sizes ranging from XS to XXXL this compression garment fits most body types. Its adjustable chest strap further helps to customize the fit to your body.

LTHA Compression Socks
LTHA’s Compression Socks can be used following leg liposuction to reduce swelling. They can also be helpful after surgical procedures across the body to improve blood flow and help prevent deep vein thrombosis. LTHA’s socks have a cushioned heel to provide added comfort during recovery.

Post-Liposuction Above the Knee Compression Garment
These compression pants are ideal following thigh and butt procedures to help reduce fluid buildup and swelling. Its full length side zipper makes putting on and taking off this compression garment a breeze, even with limited mobility following surgery. It’s high waisted design provides the support and fit that you require.