Transgender healthcare and gender-confirming surgeries are becoming more readily available to transwomen, with facial feminization among the most common procedures.
Facial feminization surgery (FFS) is a set of bone and soft tissue reconstructive surgical procedures intended to feminize the faces of male-to-female (MTF) transwomen. The goal of FFS is to help individuals with gender dysphoria feel more comfortable in their bodies – and by extension, their lives – in the gender they actually identify with, rather than the gender of their birth. MTF patients can now choose from more than 30 gender-confirming surgeries, including FFS.
Not surprisingly, many transgender people are opting to undergo these surgeries. One transwoman quoted in the 2014 landmark book, TransBodies, TransSelves, put it this way: “I consider facial feminization surgery one of my highest priorities – alongside getting my voice right. People don’t look at your genitals. Your voice and your face are how people judge you in face-to-face conversations, as well as what you see every day when you look in the mirror.”
As Jens U. Berli, an assistant professor of plastic and reconstructive surgery with the Transgender Health Program at Oregon Health Sciences University in Portland, says, “If you think about it, not getting a job or having trouble going to [one’s preferred] bathroom is largely because of how people see your face.”
So when a plastic surgeon performs FFS for a transwoman, s/he needs to be cognizant of anatomical differences between male and female faces. For example, women have fuller, shorter lips, a shorter distance from the base of the nose to the lip, and more teeth showing. A woman’s chin is narrower and more pointed, with less projection. The jaw is more rounded and not as sharply angled. Men also have far more prominent Adam’s apples than women.
What is FFS?
FFS involves modeling the face in thirds. The upper third encompanses the forehead, hairline and upper eyelids. The middle consists of the lower eyelid, nose, and cheeks while the bottom third is the chin, jaw, and sometimes the Adam’s apple. Facial reconstruction entails many bone and soft tissue procedures, but the most commonly performed are forehead reconstruction (including brow lift and eyebrow repositioning), hairline treatment or redefinition, rhinoplasty, lower jaw and chin contouring, Adam’s apple reduction, and facial hair removal/electrolysis.
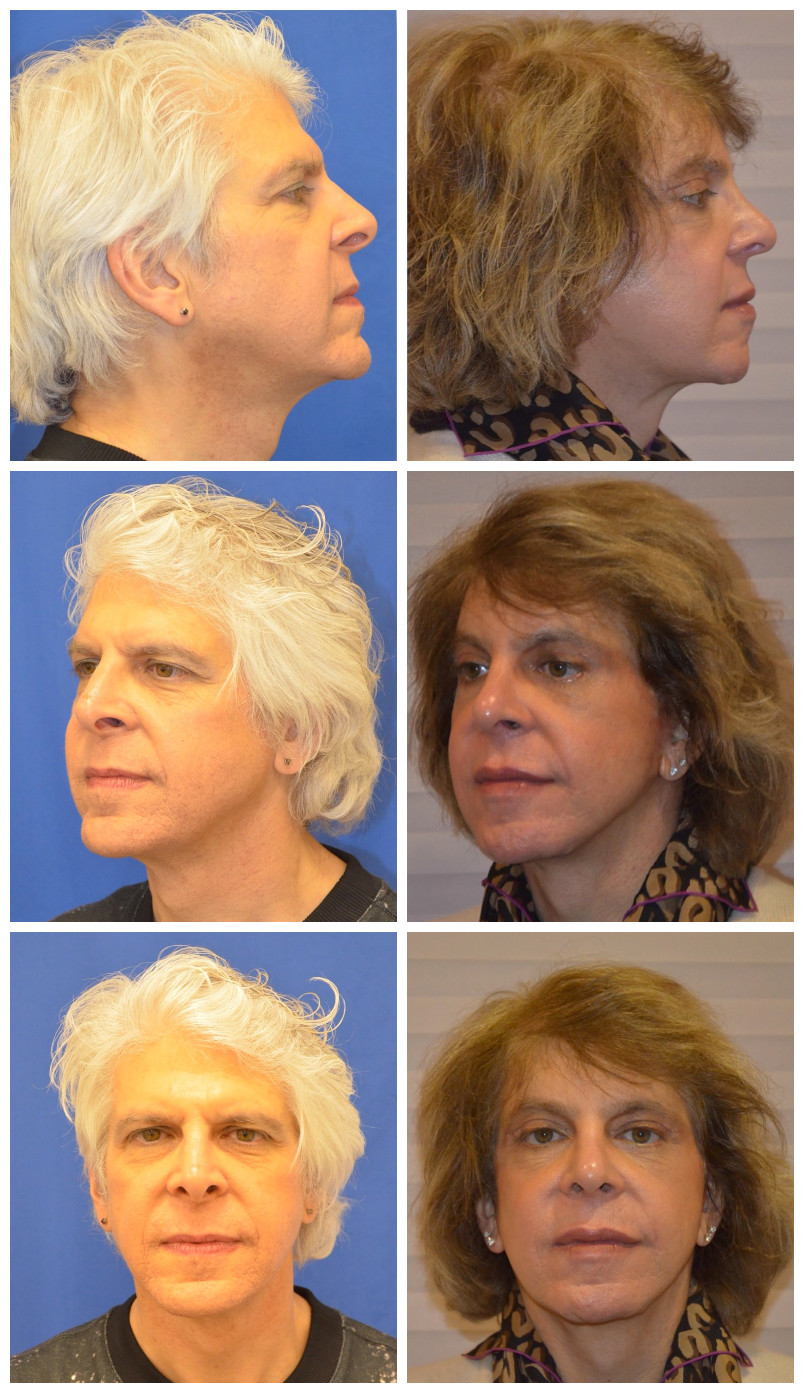
Genioplasty is the most commonly performed procedure used to reduce the prominence of the chin. The jawline can be softened with a procedure known as mandibular angle reduction. A mandibular reduction reduces the width and height of the lower edge of the jaw. Usually, these procedures are done at the same time. The surgery is performed through the mouth on the inner portion of the lower lip. The chin is then cut away from the jaw and contoured. The procedure leaves no scar because manipulation is inside the mouth. Swelling and numbness of the lip and chin can last for two weeks. A patient can usually return to work within ten days, with full recovery generally taking two-to-three weeks. Initially, patients won’t be able to chew their food and will need to go on a liquid or soft-food diet.
An Adam’s Apple Reduction, also know as a tracheal shave or chondroplasty, will minimize a person’s Adam’s apple, as the name suggests. This procedure makes a small incision just under the chin in the shadow of the neck, where it helps conceal any potential scarring. The Adam’s Apple reduction reshapes the cartilage and is typically performed in an outpatient setting.
Preparation, Timing, and Recovery
The World Professional Association for Transgender Health (W-PATH) is the widely accepted global authority that sets standards of care for FFS, as well as all aspects of transgender healthcare. You will want to be sure that your provider is following their standards of care. These standards are still evolving, so keep an eye open for any changes to the present decorum.
Before you contemplate FFS, Berli recommends you “recognize that the standard of care is that people should transition first, meaning come out to family and friends. It’s also good to be on hormones for at least a year since it changes skin quality.” Evaluation by a primary care doctor and mental health professional are also recommended.
Regarding surgery, one approach is to “perform the bone work initially, including forehead contouring, mandible contouring, and genioplasty. Then, six months later, soft tissue work can be done,” says Dr. Thomas Satterwhite, a well respected plastic surgeon with a busy San Francisco practice. “This may include facelift, blepharoplasty (to repair droopy eyelids), cheek implants, and lip lifts, etc. Every surgeon will take the approach they feel most comfortable with and guarantees predictable results.”

If a patient chooses to do the bulk of the bone work at once, it typically can take up to twelve hours in the operating room, according to Satterwhite. Additionally, he explains, patients should expect to spend one-to-two days in the hospital and plan on bedrest for at least one week, with no strenuous activity. In the first week, they will be quite swollen and bruised. Patients will require pain medication medication for about ten days and they can go back to work in about two weeks. Within three months, 80% of the swelling will go down, and the final results will be clear in about a year.
Cost, Insurance and Timing
There are multiple approaches for facial feminization surgery, depending on patient preference, logistics, and insurance coverage. “For a healthy patient, there is no reason why the majority of procedures cannot be done in one sitting,” says Satterwhite. “Because the majority of my patients are covered by insurance, getting insurance approval for multiple operations on multiple dates is exquisitely difficult.” What it comes down to are “logistics, insurance coverage, multiple times that a patient must travel, time off from work or school, and multiple recoveries, or one longer one,” Satterwhite adds.
Patients paying out of pocket might select procedures in stages to keep costs down. Costs for a full facial feminization surgery range between $30,000 to $50,000 at Satterwhite’s practice. Similar estimates are common across the United States.
Satterwhite acknowledges that patient preference is paramount in deciding how to perform the surgeries. “I’ve had some patients who insist on staging the surgery because they don’t want drastic changes all at once,” he says. Their ability to pay also clearly impacts a patient’s choice.
Patient Outcomes
Dr. Tiffiny Ainsworth, surgeon at Harvard Medical School/Massachusetts General Hospital, and Dr. Jeffrey Spiegel, plastic surgeon at Boston University Medical Center co-authored a paper on quality of life in individuals with FFS or gender reassignment surgery. Using validated quality of life instruments and patient self-reports, considered the gold standard for such studies, they reported that mental health-related quality of life diminished in MTF transgender individuals without surgery. Of the 247 patients in the study, those who had FFS or gender reassignment surgery reported better quality of life than those who did not.
A Shift Towards Facial Gender-Confirmation Surgery
The status of facial feminization surgery could soon rise, if evidence is used to update standards set by W-PATH. Review of standards of care for surgery is an ongoing process and changes are made based on the best available evidence and new studies.
Many plastic surgeons who treat transgender people favor replacing the term “facial feminization surgery” with the more precise “facial gender-confirmation surgery,” which reflects the best evidence of value. In so doing, the surgery might earn its place as being medically necessary. In fact, as transgender healthcare becomes more accepted by the greater population, “gender confirmation” is rapidly replacing more surgeries formerly described as “gender reassigned”.
Access Improving
Statistics suggest transgender healthcare and gender-confirming surgeries are on the upswing. For example, according to Mercer’s 2016 National Survey of Employer Sponsored Health Plans, gender-reassignment surgery (reshaping the genitals in the appearance of, and as far as possible, the function, to the gender a person identifies with) was covered by 43% of employers with at least 20,000 employees, a jump up from 29% in 2015. Mercer also reports that many smaller employers are considering covering it.
Gender-reassignment surgery was covered by 43% of employers with at least 20,000 employees, a jump up from 29% in 2015.
While several states have legislation in the works, transgender healthcare remains a fluid area. California’s MediCal (Medicaid) program covers hormone treatment, gender reassignment surgery, and other necessary procedures. Additionally, seven states enforce laws and policy that insurers cannot exclude transgender health from insurance policies: Massachusetts, California, Oregon, Vermont, and the District of Columbia.
Across the country, academic medical centers – especially in urban areas – are marketing new trans surgery programs or expanding older ones. As a transwoman, you may have to work with your doctors to make a case for coverage, but in 2017 and beyond, you should have a far better shot of getting it covered than in previous years.