Common in females, melasma is a pigmentary condition that’s completely benign (non-cancerous) and difficult to treat due to its typically chronic nature. With proper treatment, patients will see a dramatic improvement and in certain cases, complete resolution of their condition.
Have you noticed discolored skin on your face? You are not alone. Melasma is a surprisingly common pigmentation issue, with approximately 6 million females across the United States suffering from it.
What is melasma?
Melasma is a pigmentary ailment characterized by dark, flat patches of skin that typically appear on the face. Patients frequently complain of brown or gray patches on their forehead, cheeks, nasal bridge and upper lip, which are further exacerbated by sun exposure, pregnancy and oral contraceptives.
Although all skin types are susceptible to melasma, people with darker skin, as designated by the Fitzpatrick scale (a numerical grading system for human skin color), are at a higher risk.
Signs and symptoms of melasma
The first signs of melasma are the appearance of gray or brown patches of skin distributed in a “mask-like” assembly along the forehead, nasal bridge, cheeks, upper lip and chin. Although the vast majority of sufferers are female, the pattern is the same for everyone.
While these discolored patches of skin are neither itchy, raised or painful, they’re unattractive and because of this, patients frequently seek treatment options to rid themselves of them.
If you’re finding darker patches of skin on your face that are consistently tender, flaky, painful or itchy, be sure to consult your healthcare provider and inform them of all your symptoms as there are other, potentially more serious conditions that also cause pigment changes.
Who gets melasma: pregnancy and other factors
Those at risk for melasma may have all or one of the following contributing factors:
- Family history
- Hormonal changes
- Pregnancy
- Initiation/change of oral contraceptive or drug-eluding IUDs (medicated intrauterine devices)
- Initiation/change of hormone replacement therapy (HRT)
- Poor compliance with daily sunscreen, inadequate SPF (<30), and/or failing to regularly reapply sunscreen (especially in direct sunlight)
- Medications
- Irritation from topical treatments or skincare/cosmetic products
Up to 40% of patients suffering from melasma have a family history of pigment irregularity (e.g. their mother, sister and/or grandmother suffer from it). Check your family tree to see if others in your family have or have had this same skin condition. Doing so could help with your self-diagnosis or offer your healthcare provider some valuable information to help diagnose your condition.
Up to 40% of patients suffering from melasma have a family history of pigment irregularity.
The association of pregnancy with melasma (during pregnancy the term for the condition is “chloasma”) is still being studied, but some interesting facts have been learned from the studies that have been conducted. High levels of hormones like estrogen, progesterone, and melanocortin that increase during pregnancy are suspected of being the chief factors leading to melasma in pregnant women.
There is, however, some good news for hormone-related, female melasma sufferers: the prevalence of melasma decreases after age 50, which is believed to be related to a decrease in the amount and activity of the pigment cells in the skin (melanocytes).
In addition to birth control pills, other medications that can cause the skin to darken or encourage skin’s sensitivity to the sun leading to darkening are:
- NSAIDs (non-steroidal anti-inflammatory drugs)
- Phenytoin
- Antimalarials
- Amiodarone
- Cytotoxic drugs/chemotherapeutics
- Antipsychotics
- Tetracycline antibiotics (like doxycycline, minocycline, etc.)
Sunscreens and sunblocks are a vital piece to the melasma puzzle.
Speaking as a healthcare provider who sees a variety of medical and cosmetic conditions almost every day, one constant, regardless of the patient’s skin color, is that irritated skin is at risk of pigmenting darker than the patient’s baseline. For example, I’ve seen several patients with irritation from over-the-counter foundations, bronzers and blushes that under the right (or wrong) conditions can cause melasma.
Melasma in men
While melasma occurs less frequently in males than females, it is still common. Studies have shown that males are impacted by the same factors as females, but to a much lesser extent. Treatments for males are the same as females.
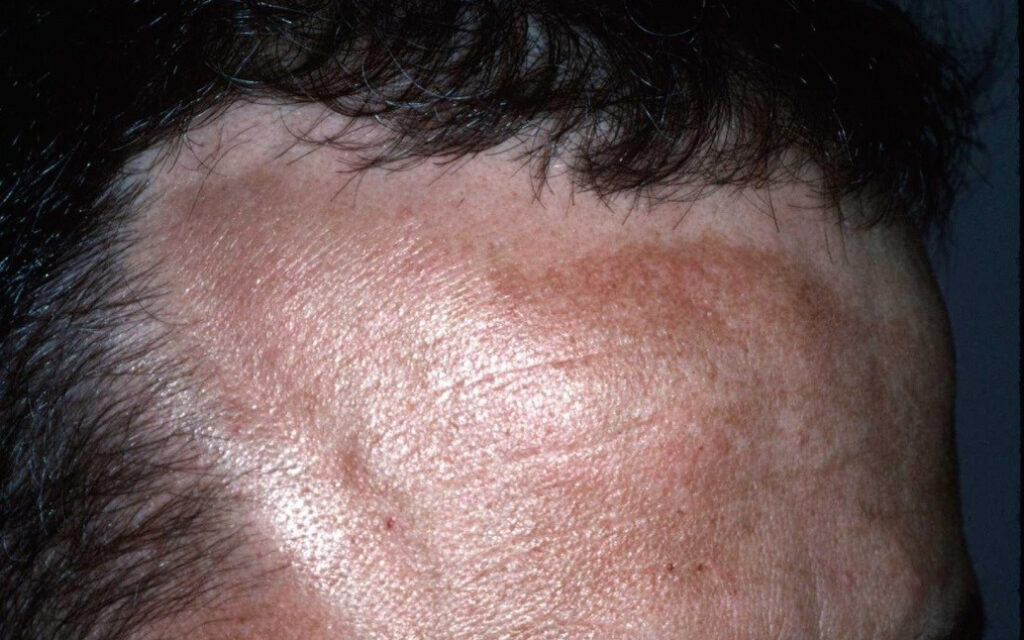
Melasma treatments and prevention
For some, time and sunscreen are all that’s required to clear up their melasma. For those individuals who don’t want to wait, there are several treatments to help expedite the healing process.
Hydroquinone (HQ, a “lightening” topical treatment, which in low doses can be purchased over the the counter and in higher doses by prescription.) is considered by the NIH to be the ‘gold standard’ of melasma treatments. However, there are newer, less demanding treatments that have proven to be very successful at treating melasma.
Prescription retinoids and corticosteroids are typically written secondarily to either HQ treatments or alone depending on the provider. Medications like Tazarotene and Tretinoin can also be found in combination with HQ and/or corticosteroids, commonly called triple therapy/triple cream.
Some patients report improvements to their melasma after using prescription Azelaic Acid or Kojic Acid. Azelaic acid has traditionally been used to treat acne rosacea and dark marks, while retinoids are used for acne vulgaris, anti-aging and dark marks.
Common side effects of retinoids are dry, irritated skin that leads to an itching or burning sensation when not properly protected and can lead to hyperpigmentation (darkening) of the skin.
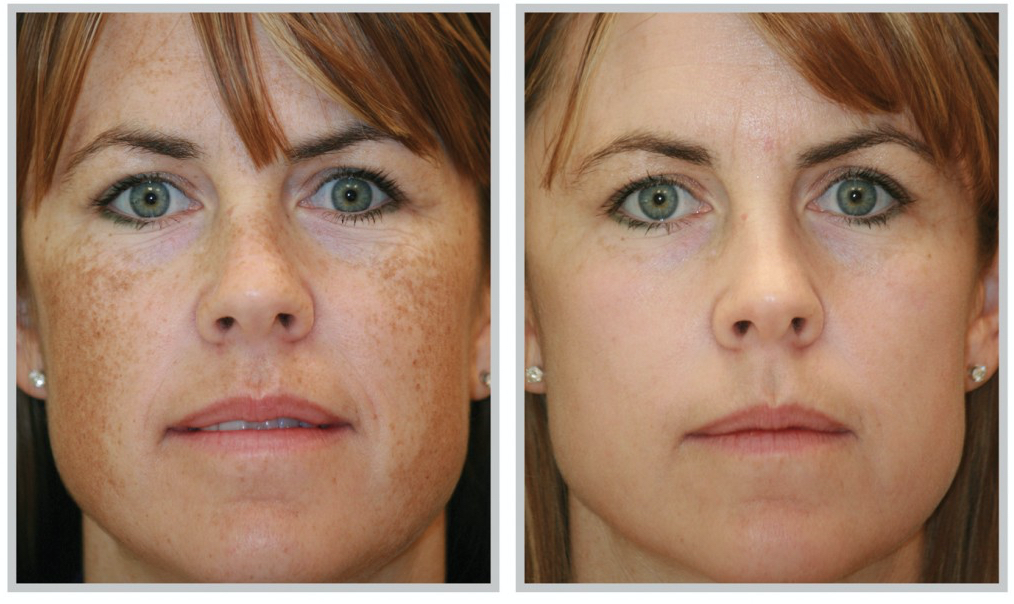
There are many procedures that can easily be performed with great results at your dermatologist or cosmetic surgeon’s office. Be sure to fully vet your provider on your skin type, risks and post-procedural care, so that you are at minimal risk of adverse reactions or worsening your condition. Such procedures include chemical peels and dermabrasion.
Ultimately, preventing melasma is key – as is maintaining a successful treatment regimen. Regularly reapplying sunscreen is necessary to protect against the sun’s rays leading to hyperpigmentation. The American Academy of Dermatology (AAD) recommends an SPF of 30 (while also being waterproof, which on a day-to-day basis may not be necessary) reapplied every 2 hours to provide continued protection.
An SPF of 30 provides 97% protection from the sun’s harmful rays, while 45 SPF provides 98% protection. It’s presently impossible for any SPF to provide 100% protection from the sun, so don’t believe the hype!
Regardless of gender, the prevention and reduction in exacerbation of melasma requires one common element: sunscreen (of 30 SPF or more with reapplication). You can protect the face, arms, neck, etc. with daily use, and help to maintain results you may invest in either with your time, finances, or both. Above all, protect yourself and your investment in healthy skin.
Top Melasma Treatments: Pros and Cons
Not everyone needs treatment for melasma; in many cases it goes away on its own. However, in some cases melasma can last for years on end — or never go away. The American Academy of Dermatology recommends the following treatments if melasma does not fade away on its own and for women that want to keep taking birth control pills:
Hydroquinone (HQ) in cream, lotion, gel, or liquid form
Pros: Very effective (considered the gold standard of melasma treatments by the National Institutes of Health); you can obtain some hydroquinone products without a prescription.
Cons: These products don’t have as much hydroquinone as products your dermatologist can prescribe.
Prescription tretinoin and corticosteroids prescribed by your dermatologist
Pros: Can be prescribed as a complement to hydroquinone; added boost of prescription medication can help some patients that don’t respond to hydroquinone alone; “triple cream” (hydroquinone, tretinoin, and a corticosteroid in one cream) is also an option.
Cons: Can cause dryness and irritation that leads to itching or a burning sensation if treatment site is left unprotected; can cause darkening of the skin (hyperpigmentation).
Other topical medicines (azelaic acid, kojic acid)
Pros: Can help to lighten melasma.
Cons: Can cause an array of side effects, from mild itching to a dangerous, life-threatening allergic response. As a result, it is imperative that you speak with your doctor before using azelaic acid or kojic acid, and possibly have a skin patch test to make sure you are not allergic.
In-office procedures (chemical peel, microdermabrasion, dermabrasion)
Pros: Can be helpful if a topical medicine does not get rid of your melasma.
Cons: Costs more; can’t be performed at home (a dermatologist or other qualified physician needs to perform it). New skin problems can crop up if the person who performs the treatment does not take into account the patient’s skin type.