“A kiss,” said the romantic hero Cyrano de Bergerac, “is a rosy dot.” During de Bergerac’s era, rosy cheeks were seen as a sign of health and beauty. However, an overly warm glow in the cheeks can also be a symptom of rosacea, a chronic skin condition that causes redness and irritation in the face.
What is rosacea?
Rosacea is a fairly common condition, affecting approximately 16 million Americans from all walks of life, and some 45 million people worldwide.
One famous rosacea sufferer was Rembrandt, who painted self-portraits throughout his lifetime. Even from a young age, signs of rosacea appear on his cheeks and nose. Ann Chubb’s book, Royal Fashion and Beauty Secrets, reports that the late Princess Diana had rosacea, while her son, Prince William, also has a rosy face prone to occasional flare-ups. Former President Bill Clinton has rosacea that becomes more apparent under stress.
The condition is easy to misdiagnose. People with rosacea frequently make the mistake of thinking they have acne. Recalling their teenage years, they buy over-the-counter acne treatments only to find the products can irritate their skin or even exacerbate the problem.
However, much like acne, rosacea is a chronic, possibly inflammatory, condition. Among fair-skinned people, it produces redness that periodically intensifies (erythema) over the face and various other parts of the body. In dark-skinned people, the redness may appear as a darker shade of brown, or even purple.
A second symptom that may appear by itself or with the erythema is a change in the texture, color and thickness of the skin (phymatous changes).
According to guidelines outlined by the National Institutes of Health (NIH) released in February, 2017, either one of these two symptoms is sufficient to diagnose rosacea. The condition can also cause a range of other symptoms, including pimples, spider veins, and itchy, red eyes. The severity of these symptoms varies from patient to patient.
What type of rosacea do I have?
Up until very recently, rosacea was divided into four main sub-categories:
- Erythematotelangiectatic rosacea
This is the most common type of rosacea, causing redness in the cheeks, lower nose and forehead. Spider veins on the cheeks or nose are also included in this category, although they are not always present. In its mildest form, the red color may not be striking except during bouts of facial flushing.
- Papulopustular rosacea
This variation is also sometimes called acne rosacea because the red skin is accompanied by pimples and pustules. The term should be avoided, however, because acne and rosacea do not share the same cause. Flare-ups of this type of rosacea may be accompanied by burning or stinging sensations.
- Ocular rosacea
Rosacea may be accompanied by a variety of ocular symptoms including blood-shot, watery eyes, itching, the feeling that something is in your eye, sensitivity to light, and blurry vision. If left untreated, the eyes can become permanently damaged.
- Phymatous rosacea
The skin becomes thicker, marked by irregular nodules and swelling. Phymatous rosacea is most commonly observed in the nose, but can also appear on the ears, cheeks or forehead. Deep red coloring and spider veins can also accompany this condition.
By simply reading the descriptions of these variations of rosacea, it’s evident that there is an extensive overlap of symptoms, and that not all symptoms need be present in a defining type. Ocular rosacea, for example, may have many symptoms or only a few, while erythematotelangiectatic rosacea is present to some degree in almost every instance of the condition.
The adjustment to the 2017 guidelines for diagnosing rosacea are an acknowledgement that the earlier categorization was not truly successful in sorting symptoms or causes. The new guidelines recommend treating each case of rosacea according to its own set of observable symptoms.
How can I tell if I have acne or rosacea?
Although acne is considered a problem for adolescents and rosacea is associated with adults, this stereotype doesn’t always hold true. Teenagers with acne may be told by their doctor that they also have rosacea, or appear to be at special risk of acquiring rosacea later in life, and as such should take precautions now. Adults with rosacea may sometimes have acne as well.
As the two conditions have different causes and necessitate different treatments, you’ll definitely need a doctor’s diagnosis to be certain of which disease is afflicting you.
Other skin conditions sometimes confused with rosacea include eczema, which can arise from an allergic reaction, and cutaneous lupus.
What are the visible symptoms of rosacea?
Rosacea is quite a common skin condition — almost 10% of American adults are believed to suffer from it.
It is most easily observed on people with white skin. Darker skin can mask the condition’s presence, causing it to be under-reported. Women more commonly get the periodic intense reddening, while men are more apt to see changes in their skin texture. It may affect people of any age but is most common among the middle-aged (40-60). Symptoms include:
- Facial redness
The most common symptom is a red glow to the face (cheeks, forehead, nose or chin). From time to time, this rosy hue can flare up into a more intense red. When appearing around the eyelids, it is sometimes confused with adult blepharitis or allergic conjunctivitis. Occasional flushing of the face need not indicate rosacea, but recurring episodes are common in many clinical cases.
- Spider veins (telangiectasias)
Small connections between the arteries (which carry blood away from the heart) and veins (which bring blood back to the heart) can become malformed and visible as a series of small red dots on the surface of the skin. Other symptoms may mask the spider veins so they only become noticeable after these other symptoms have been successfully treated.
- Hard pimples (papules)
The appearance of pimples on the face can lead people to think they’ve somehow developed acne, even though they’re well out of their teens and may never have experienced acne when they were teenagers.
Although adults can have acne, the pimples associated with rosacea are different from acne pimples. Acne is caused by dead skin cells and oils that build up and clog the pores. Classical acne treatments (topical rubs placed on the skin) can actually make rosacea-based pimples more irritating.
- Softer pimples containing pus (pustules)
These pimples may only be tiny pinpoints but the quantity of pus produced can be alarming. Pimples and pustules may be accompanied by a burning or stinging sensation.
- Dry skin
Almost half of all rosacea patients are believed to have dry skin. Rosacea patients with dry skin should be especially vigilant about applying moisturizer every day. Other skin conditions (e.g., dandruff, oily skin) may also occur with rosacea.
- Strawberry nose (rhinophyma)
Thickening skin with nodules (phymatous) is another primary symptom of rosacea and often found on the nose. The thickened skin may also appear on the chin, forehead, ears, or eyelids. This condition is often a late development of uncontrolled rosacea with pimples or pustules.
- Sensitivity to facial makeup
Rosacea can make the skin more sensitive, causing it to react strongly to facial makeup such as foundation.
- Red and watery eyes
The eyes may become dry, irritated, and watery. Other issues that can arise with the eyes may include frequent styes or infections, redness, and sensitivity to light (photophobia). Sometimes the eyes may feel as though they have grit or another foreign body in them.
It is especially critical to see a doctor if the rosacea affects your eyes. Persistent rosacea can eventually damage the cornea and even lead to blindness.
Rosacea can also lead to an inflammation of the inner edge of the eyelid (posterior blepharitis). This condition causes irritated, itchy eyes and should be treated by a doctor.
- Demodex
One of the normally beneficial life forms living on the epidermis is a tiny, nearly invisible mite called demodex.
Normally, demodex is no cause for alarm, but some studies have found that these microorganisms are unusually plentiful during rosacea flare-ups. They may be especially important in producing pimples and pustules that often accompany rosacea, and some treatments are expressly designed to reduce the presence of demodex.
- Damaged blood vessels
Some of the secondary symptoms associated with rosacea (e.g., spider veins) are known to arise from damage to the vascular system (blood circulation). These symptoms are not always present in rosacea, and may only be contributing factors in certain clinical cases rather than primary causes of the disorder. Blood vessels may swell, making the red visible through the skin.
What causes rosacea?
Rosacea is a symptom of skin damage, although the cause of that damage is uncertain. Reassuringly, rosacea is not contagious. If you have rosacea, there is no need for friends or acquaintances to worry that they might catch it from you.
It’s possible that due to the range of symptoms and the differences in treatment success, rosacea has more than one cause. Despite the uncertainty, there are a few known triggers:
- UV light
Ultraviolet light from the sun can penetrate through clouds. Even on an overcast day, this light reaches your skin. It is known to cause skin damage, and some medical authorities postulate that the damage brings capillaries in the hypodermis closer to the skin’s surface, or even close to the bottom of the epidermis. This change would explain both the reddened skin and a secondary symptom, small red dots sometimes called spider veins.
- Immune system disorders
One popular belief is that a hypervigilant immune system may cause rosacea flare-ups. Normally, the immune system kills and removes alien invaders, but sometimes it overreacts and damages the body it is supposed to protect. In this case, the skin itself may be attacked.
This account would explain the red coloring in the skin as part of an inflammatory response to halt a non-existent invasion. It might also explain why, even after rosacea has been successfully treated, there are periodic flare-ups. An overactive immune response might trigger a reaction.
One particularly relevant part of the immune system is the mast cell, a type of white blood cell. Studies of rosacea patients indicate that they have more than the normal amount of mast cells. This could indicate, however, that mast cells resist rosacea rather than cause it.
One interesting study discovered that if mice with mast cells are injected with material from a patient with rosacea, they begin showing symptoms of rosacea. If the mice do not have mast cells, an injection with the same material does not produce any symptoms. With further study, it’s hoped the mechanisms that provoke rosacea will be better understood and a target for treatment identified.
- Genetics
There is some evidence that supports the premise that rosacea runs in families, although no gene or combination of genes has been identified as making the disorder more likely.
A genetic effect is often indirect. For example, a hereditary predisposition might make a person more susceptible to skin disorders caused by ultraviolet light. In that case, the rosacea would not be directly inherited, but a greater susceptibility to the disorder would be passed down through the generations.
- Alcohol
The three causes outlined above are all possible explanations for the reddish color of the skin. However, no concrete hypothesis has yet emerged to explain the excess tissue (phymatous) that constitutes the second primary symptom of rosacea. There is, however, a popular folk explanation: long-term alcoholism.
The logic is simple: sometimes alcohol causes a person’s face to redden, and eventually the drinker’s face might remain in a permanent flush. Alcohol can indeed be one of the triggers of a rosacea flare-up, except many alcoholics never get the excess tissue, while non-drinkers occasionally do.
As a general rule, refraining from alcohol or drinking in moderation is the most prudent guideline to follow, even if phymatous is not a sign of excessive drinking.
RELATED: Treating Rosacea — FDA Approved Medications and Their Side Effects
Common rosacea triggers
While the causes of rosacea remain uncertain, the triggers that lead to flare-ups of the condition are understood. Triggers bring blood to the face; drinking wine represents one such example. Rosacea flare-ups can also accompany menopause, or be a symptom of caffeine withdrawal.
The National Rosacea Society has surveyed over 1,000 patients and found a long list of triggers. Most of them were reported by a minority of patients, but the following five were common to more than half of the patients surveyed.
The best technique to avoid triggers is to keep a record of your flare-ups, noting the weather, your emotional state, any recent activities and the foods you’ve eaten. If a pattern emerges, you’ll know which triggers to avoid.
- Weather conditions
Exposure to the sun is the most commonly reported trigger. It’s recommended patients wear broad-brimmed hats and apply sunscreen regularly. Strong winds and hot weather in general will trigger flare-ups in many cases.
- Emotional state
Another trigger almost as widely reported as sun exposure is emotional stress. This trigger can be especially upsetting to patients at work where the rosacea flare-up can even increase the stress. It can also complicate an already embarrassing social situation when the rosacea suddenly reddens a face, signalling to everyone just how upset the person is.
- Lifestyle factors
While not as common as the sun or stress factors, lifestyle can also trigger flare-ups. Exercise, alcohol and hot baths can actually intensify rosacea.
Of course, people who find that exercise triggers intense rosacea shouldn’t stop exercising. Instead, they only need to change their exercise programs so they become less intense. Stay well hydrated by drinking plenty of water, and when the workout is finished be sure to cover your head with a cool, wet cloth.
- Foods
Many people report how certain foods can trigger a flare-up. While trigger foods varied among sufferers, spicy foods were found to be the most common dietary trigger.
- Medications
Rosacea flare-ups can sometimes be a side effect of certain medications. If that happens, don’t stop taking the drug, but speak with your doctor and see if a substitute medication is available.
Can rosacea be cured?
There is no cure for rosacea, but its symptoms can be minimized and in some cases, even permanently eliminated. Once the condition is treated, patients will need to adjust their habits and lifestyle to keep flare-ups to a minimum.
Treatment depends on the symptoms displayed. If a patient displays pimples or pustules, these should be treated first. They can spread and also tend to cause many people the most concern about how they look. Problems with the eye are also an area of concern and call for prompt treatment. If there are changes to the skin — thick, nodules on a rosy skin — those should be examined promptly as well.
The Internet is rife with information devoted to home and herbal remedies for rosacea. Most of them have not been scientifically tested nor approved by the FDA and as such, are not listed here. Your doctor, however, may know from clinical experience if a particular natural remedy may be beneficial for you and as such recommend it.
Treating rosacea pimples and pustules
The principal treatment for the lesions commonly associated with rosacea are ointments that are rubbed on the skin. There are many of these medications, some more effective than others, but a treatment that is effective for one person may not help another.
Patients should be prepared to try more than one ointment to learn which is the most effective for them personally.
- Azelaic acid (Finacea)
In gel form, this is used as an anti-inflammatory medication. It can darken skin where it is applied (hyperpigmentation) and should therefore be used cautiously by darker skinned patients. It should not be used around the eyes or mouth. Apply twice daily. For fairer-skinned individuals, there is evidence that it is effective.
- Benzoyl Peroxide (BenzEFoam, MaxClarity, PanOxyl)
This is a gel used chiefly to treat acne, but one recent study found that the 5% benzoyl peroxide solution does in fact provide some relief for rosacea. It should be noted, however, that this product is not a first line of defense when treating rosacea pimples. Another acne treatment, Clindamycin phosphate, was found to provide no relief whatsoever for rosacea.
- Isotretinoin (Sotret Oral)
Ingested orally, this drug was originally introduced to treat acne but has also been found to provide some relief from rosacea.
- Ivermectin (Soolantra)
This cream is an anti-parasitic medication that is also available orally, however, only the cream should be used to treat rosacea. It’s used to reduce the presence of demodex mites and should not be applied around the eyes. Use 1% Ivermectin cream once daily.
- Metronidazole (Metrogel)
This gel has long been the most popular treatment for rosacea pimples and is still considered highly effective. Ivermectin is judged slightly more effective, but is also more expensive. After applying the gel, wait half an hour before using cosmetics.
Treatments for redness and spider veins
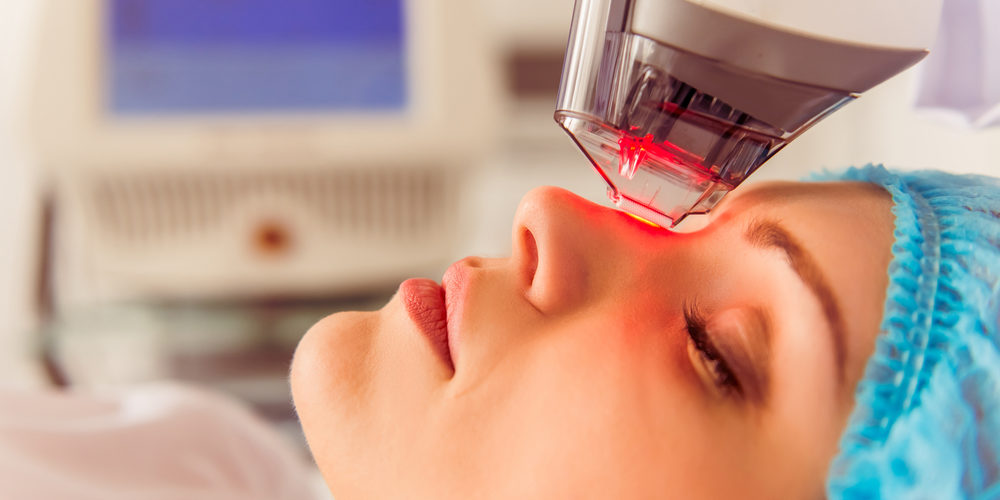
The redness — also known as erythema — may result from capillaries carrying blood close to the surface of the skin. Medications can temporarily reduce this activity, but for a longer-lasting solution there is laser surgery. The objective is to seal off the capillaries just below the skin so the deep redness is reduced or possibly even removed.
- Brimonidine (Mirvaso)
This gel is effective in reducing mild to severe erythema. Patients typically find that it works well, although the effects wear off after 12 hours. A sudden flushing may occur some 3 – 4 hours after application, but tends to be no more common than a typical flare-up without the gel.
- Clarithromycin (Biaxin)
This antibiotic has been found to have the side-effect of reducing erythema.
- Oxymetazoline hydrochloride (Rhofade)
This 1% active ingredient cream that showed promise when tested on patients with mild to severe erythema. Use a small dab of the cream, covering the face and forehead while avoiding the eyes and mouth.
- Pulse dye laser
This treatment is used for both the redness and spider veins associated with rosacea. Pulse lasers produce flashes of light that create a mild, pin-pricking sensation on the skin. For redness, the laser is moved across the entire affected area, which may be most of the face and forehead, and can require several sessions. For spider veins, the session tends to be shorter as the laser only needs to focus on the affected area.
Recovery takes a few weeks and can include swelling and bruising. Patients who are unprepared for these first results can become quite alarmed. After three or four weeks, however, the healing progresses enough for beautiful, long-term results to become visible. Spider veins disappear and the redness is reduced to a pinkish glow.
- Broad Band Light (BBL)
BBL has been found to be another effective treatment for rosacea. This particular technology is a non-ablative procedure, and works by emitting bright lights at high energy frequencies. The treatment stimulates the skin to increase collagen production and breaks up unevenness in the complexion, contributing to a more balanced skin appearance. The thermal energy of BBL also targets and removes the vessels that provoke skin redness, which is the main symptom of rosacea.
For optimal results from BBL, a course of four to six treatments is required. These sessions should be delivered several weeks apart. However, your dermatologist or surgeon will most likely examine your case and formulate a treatment plan uniquely suited to the severity of your case. Although BBL may not completely eliminate rosacea, the treatments can offer long-lasting improvements. In addition, this laser treatment is virtually painless and has minimal side effects.
- Intense Pulsed Light (IPL)
IPL is a non-invasive treatment that uses multiple wavelengths of light to treat prominent blood vessels on affected areas of the face. The light emitted is absorbed into the skin and the capillaries that cause facial redness are destroyed. Overall, facial inflammation, flushing and red patches are diminished.
IPL works most effectively as a course of four to six initial treatments, delivered a month or more apart. There may be some residual facial redness following the session, but this subsides after several days. There is virtually no downtime, and the patient can resume normal activities immediately.
While IPL may not permanently eliminate the appearance of rosacea, the condition can be successfully contained and managed with regular IPL maintenance treatments.
RELATED: Laser Treatments for Rosacea — Frequently Asked Questions
Treating eye irritation and redness
If you’ve been diagnosed with skin rosacea, ask your doctor whether you should undergo periodic eye exams. A specific treatment to help control ocular rosacea may also be required.
- Artificial tears
Eye lubricants are available over the counter at most pharmacies. Use as often as necessary throughout the day. For many people, these products serve as the first line of defense in getting rid of red, itchy eyes.
- Cyclosporine (Restasis)
Cyclosporine is available as an eye drop or as a tablet, but one study found that the eye-drop form is more effective in treating rosacea. The product was originally developed to increase the tearing of dry eyes and its use in treating rosacea is still somewhat experimental.
- Metronidazole (Flagyl)
This is the same medication used as a gel on rosacea pimples and pustules, but in this form it is swallowed as a tablet. Alcohol cannot be consumed while taking this medication. Rare but severe side effects (nerve damage, seizures) make it an unlikely first choice as a medication.
- Steroids
Although steroids placed on the eyelid can have beneficial effects, it is a last resort measure only, and must be discontinued as soon as possible. Steroids can do permanent damage to the cornea and increase the erythema on the face.
- Tetracycline (Oracea)
The class of antibiotics containing tetracycline, doxycycline and minocycline are the most common treatment for the eye problems associated with rosacea. (Note: antibiotics are not recommended for treatment of rosacea that is not associated with eye symptoms.)
It may be surprising to see an antibiotic prescribed, as rosacea is not caused by bacteria, but in this case the drugs have a secondary effect that protects the cornea from damage. The dosage is much lower than that prescribed for antibiotic purpose. Once the symptoms are cleared up, patients can take an even smaller dose to reduce the chances of a flare-up. This minimal dose medication may continue indefinitely.
Surgical treatments for strawberry nose
A bulbous, red nose is fairly rare, but inspires rumors of alcoholism and as such can be a significant source of social discomfort. Treatment for the nose does not address other symptoms of rosacea, which should be treated once the nose has been restored to a more typical shape and size.
- Electrosurgery
There are multiple techniques that use electricity to make removal of tissue easier. The electrical current first destroys tissue before the surgeon removes it. When used to treat a nose or other parts of the face with thickened, rosy skin, surgeons use a high-frequency electric current that causes heat damage to the unwanted skin. This technique is especially useful for reducing skin bulk without any causing any significant blood loss.
The surgeon uses an electric loop like a scalpel, drying and scraping off the layers of skin. Thick, bulbous growths can be removed in this manner, shedding minimal blood. It’s also a relatively painless procedure because medication is used to numb the skin. In cases of very large growths, the procedure may take several sessions, allowing a few weeks between sessions to permit healing. The final result is a shapely nose without scar tissue.
Patients with implanted electrical devices like pacemakers, cochlear implants, etc. should thoroughly discuss this procedure in advance with their surgeon. Electrosurgery may cause problems with the normal functions of such devices, which could lead to a potentially dangerous situation.
- Carbon dioxide (CO2) laser surgery
This technique is used to treat moderate to severe cases of rhinophyma. It’s similar to electrosurgery in the sense that it removes tissue with limited blood loss.
A local anesthesia is applied to numb the nose while patients wear blinders to protect their eyes throughout the procedure. The laser is then used to remove skin tissue layer by layer. The skin is vaporized and does not need to be scraped away. A surgical assistant vacuums away the vapor as it emerges. The CO2 laser produces a continuous bet allows for rapid results. Healing takes several weeks. The treatment does not resolve the erythema.
Darker skinned patients should take note that even darker points of pigmentation may result from this surgery. That said, normal pigmentation can almost always be restored through bleaching therapy, or by simply waiting for 3 – 4 months.
CO2 lasers are excellent tools that provide pleasing results over time. Patients must realize that they will not immediately emerge from surgery and be delighted with what they see in the mirror. Depending on the procedure, the results may appear non-existent — or worse. The dark pigmentation can be especially alarming, while the strange and ugly nose shape after carbon dioxide laser surgery is also disquieting.
Four weeks on, however, the results can suddenly seem miraculous, and after six weeks patients are generally delighted with the outcome. For this reason, it is advisable to not schedule your surgery just before an event where you want to look your best. Wait for at least a month and a half.
How much do rosacea treatments cost?
Insurance should cover the cost (with perhaps a co-pay) of your initial visit to your primary care physician for a diagnosis. Any topical medications or tablets prescribed will depend on the details of your pharmaceutical plan.
A survey taken by the National Rosacea Society in 2014 found that 72% of those surveyed reported their insurance plans covered the topical and oral medications. This coverage doesn’t mean that the medications are free, but prices are reduced.
The laser and electrosurgical treatments are both fairly long-lasting but more expensive than other approaches. The survey data was unclear about these procedures because most of those surveyed didn’t know whether their insurance covered them or not.
Health insurance companies are reluctant to cover surgery they consider cosmetic, and many patients find their insurance lacking when it comes to covering rosacea treatments.
The surgery is usually performed on an outpatient basis without the need for an anesthesiologist. There will be an assistant whose costs must also be covered. Laser treatments can require several sessions, with each session including a basic, office-use price. The laser surgery itself is in the range of $250 to $600 per session. Note, however, that treating rosacea growths on the nose, ear and other parts of the face is generally more expensive.
What should I do to maintain skin health?
Once treatment has reduced or eliminated symptoms, patients should develop a daily routine to manage their condition and keep flare-ups to a minimum.
- Manage your diet
The idea is to eat healthy, enjoyable foods without triggering a rosacea flare-up. Almost every rosacea sufferer has some trigger foods, but these differ from case to case.
As a general rule, avoid spicy foods and acidic foods (e.g., citrus fruits, pineapples, grains, and sugar). Avoiding sugar is particularly difficult as it’s included in almost all processed and fast food. Pay close attention to how much sugar you are actually consuming. Keep your skin properly hydrated and drink water throughout the day.
- Treat your face gently
Wash with a soft soap. A useful cleanser is Sulfacetamide 10%-Sulfur 5%. Use hypoallergenic cosmetics. Rub moisturizers into your skin every day. Men should use moisturizers before they shave, and they should try to use an electric razor. If you prefer disposable blades, change the blade every week. Reapply moisturizer when you have finished shaving.
- Guard against sun damage
Apply sunscreen daily to your skin. The sunscreen must contain zinc oxide to be truly effective, although titanium dioxide is also acceptable. SPF measures blockage of ultraviolet radiation. SPF 30 blocks 97% of the rays, which is sufficient for most people.
The noon sun is the most damaging, and you should ensure you use sunglasses, a wide brimmed hat and a long sleeved shirt when you go out.
- Protect your eyes
Keep your eyes moist and clear. Use eye drops (artificial tears) when first waking up in the morning, as needed during the day, and just before going to bed for the night.
To avoid irritating your eyes, wash your hair with baby shampoo.
Avoid direct sunlight by wearing a hat and sunglasses. The sunglasses should block 100% of ultraviolet light. Wraparound glasses are the most effective for protecting against side exposure.
- Adapt your routine to colder weather
Summer poses an obvious risk with all that sun, but winter carries risks as well. When outdoors in a chill wind, use a scarf to protect your face and don’t forget to keep using sunscreen. Indoor heaters may be tempting in winter, but stay far enough away from the heat to avoid triggering a rosacea flare-up.
Use a humidifier to keep your skin from drying out.
When should I see a doctor?
There is no blood test or other test for rosacea, but your doctor can diagnose the disease on the basis of the collection of symptoms you display.
You should especially seek advice if you notice that a normally rosy complexion has turned a deeper shade of red. This change may indicate that your rosacea has advanced to a more severe stage and other symptoms may develop. Your primary care doctor may not be able to recommend particular treatments or management programs, but can recommend an appropriate specialist.
Mild rosacea with a simple reddening of the cheeks and forehead may seem trivial, but there are good reasons for having a doctor examine it. With time, rosacea tends to become more severe; the rosy color can deepen and other symptoms may appear.
It’s never too early — or too late — to start taking care of your skin in order to prevent the exacerbation of rosacea.