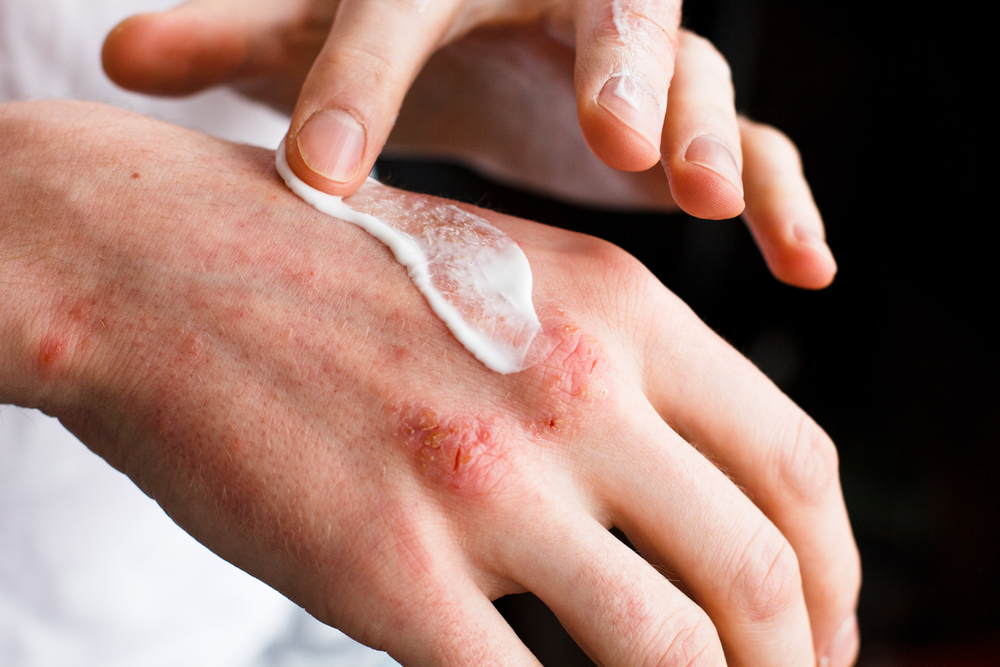
- Topical corticosteroids are synthetic medicines used to control skin conditions such as eczema and dermatitis.
- Side effects can generally be avoided by following your physician’s directions on the correct use of these medicines.
- Boosting your immune system can help reduce your dependency on corticosteroids.
In today’s world, our skin is faced with a continual assault of chemicals, bacteria, infections, and UV rays. As a consequence, we are increasingly guarded about protecting the well-being of our largest organ.
But in spite our best efforts, environmental agents, stress, and allergies can still trigger skin irritations that require treatment.
If you’re already living with a skin condition like dermatitis, eczema, psoriasis, itching, or a general rash and have paid a visit to a dermatologist, you know how this treatment scenario usually plays out. You receive a prescription for a topical cream containing a corticosteroid that typically provides instant, short-term relief for the itching and inflammation.
These drugs may be fast-acting, but they also pose certain risks. Here’s what you need to know about the potential side effects of corticosteroid use.
What are Topical Corticosteroids?
The production of natural corticosteroids hormones occurs in the outer layer of the adrenal glands. Topical corticosteroids, on the other hand, are synthetic and provide potent anti-inflammatory relief. They are effective medicines, but also come with side-effects that include suppressing your immune response.
Boca Raton, FL, dermatologist Dr. Jeffrey Fromowitz says the use of topical corticosteroids is universal. “They are a mainstay in our treatment armamentarium.” While some regard such topical treatments as miracle creams, Fromowitz warns that they also come with risks and as such their use needs to be supervised by a reputable board-certified dermatologist.
”Topical steroids come in different strengths”, explains Fromowitz. “As potency increases so too does the risk profile. High potency topical steroids can cause atrophy or thinning of the skin. Furthermore, when prescribed for the wrong conditions, steroids can make matters worse.”
Common Side Effects
As with most prescription medicines, corticosteroids come with potential risks and side effects. The degree to which these side effects manifest is dose-dependent, meaning the more powerful the dose and the longer you take it, the higher your risk.
- Atrophy — Skin atrophy can occur after prolonged use. Steroids inhibit collagen production, resulting in thinner, fragile, more transparent skin.
- Epidermal barrier disturbance — When atrophy occurs, damage to the skin’s protective barrier allows allergens, bacteria, and toxins deeper access to your epidermis. This can result in rashes and skin irritations.
- Delayed wound healing — Thinning skin also results in the inhibition of the healing process.
- Telangiectasia — Steroids contribute to the increase in both the size and number of small blood vessels on the skin. As a consequence of skin atrophy, blood vessels in affected areas become increasingly visible.
- Steroid rosacea — Reddening of the nose, forehead, cheeks, and chin occurs as the skin thins and the size and number of blood vessels increases.
- Acne — Although short-term use of corticosteroids can suppress acne, prolonged use may spark a flare-up.
- Hypertrichosis — This condition causes the growth of small, thin, short hair on the cheek and upper lip.
- Hypopigmentation — This decrease in the pigmentation or coloration of the skin occurs because steroids inhibit the production of melanin. Melanin is a natural substance responsible for skin, hair and eye color.
- Infections — Many corticosteroid users experience bacterial skin infections as well as fungal and yeast infections.
Rules for Using Topical Corticosteroids
Follow your physician’s advice regarding the appropriate steroid cream that is right for you:
- Adhere to the instructions regarding the proper frequency and duration of their use.
- Do not end steroids abruptly. Instead, reduce the strength and frequency of the steroid treatment as your skin condition improves.
- Contact your physician if you begin experiencing side effects that include: burning sensations, skin irritations, redness, and itching.
Hollywood, FL, dermatologist Dr. Todd Minars says that to help patients avoid side effects when taking strong corticosteroids, a rotation is suggested. “Dermatologists often advise a combined treatment that alternates between the less powerful topical inhibitors that don’t contain steroids and the strong stuff. For example, weekends with steroids and weekdays with the milder stuff.”
Corticosteroid Withdrawal
There is little risk of encountering withdrawal symptoms when corticosteroid’s are used properly. However, if they are used frequently for an extended period of time, it is possible to encounter several issues. Beyond an increased chance of side effects, prolonged use can lead to withdrawal symptoms when people choose to stop using the corticosteroid.
Skin redness occurs in essentially all cases of corticosteroid withdrawal. Also known as erythema, this common skin issue fades over time, and is mainly a cosmetic concern. This redness is often patchy, however, while less common, some experience a general redness along their arms.
More significant issues like a burning sensation are also possible. Occurring in roughly 65% of withdrawal cases, it can range from a slight stinging to a painful burning feeling. Over half of withdrawal cases also cause “elephant ear” wrinkles — a wrinkling that can lead to skin bunching up around the elbows and knees.
Mood swings and trouble sleeping have also been associated with withdrawal.
Following a physician directions on proper quantities and discontinuing use as direct, are the best ways to avoid these issues.
Alternatives to Corticosteroids
For skin conditions like eczema and psoriasis, there is no cure. But there are ways to boost your immune system and control flare-ups, thereby reducing your dependency on corticosteroids.
Your skin is a crucial component of your body’s immune system, providing a front line defense against bacteria, viruses, microbes, and chemicals. The following suggestions can help you minimize skin irritations while maximizing its protective potential.
1. Quit smoking
Smoking cigarettes causes premature skin aging, increased infections and delayed wound healing. Smoking also contributes to skin disorders such as psoriasis and lupus. So do yourself a huge favor and quit.
2. Drink plenty of water
Your skin requires hydration.To keep your skin invigorated make sure you are consuming water throughout the day. Substitute alcohol, caffeine, and soft drinks that dry out your skin with refreshing H2O.
3. Exercise
Stress can trigger psoriasis, rosacea, eczema and cause hives. Stress management is key to avoiding unwanted flare-ups. And one of the best ways to manage stress, of course, is through regular physical exercise.
4. Diet
A balanced diet rich in vitamins and minerals helps prevent skin problems.
Avoiding fast food, hormone-laden dairy products, chocolate, french fries, and processed meats can contribute to healthier skin. And if you’re prone to allergies, stay away from refined grain products made with wheat, conventional dairy, shellfish, and peanuts.
Do include foods that have an abundance of omega-3 fatty acids. Consuming food rich in omega-3 contributes to smoother, younger-looking skin and a noticeable reduction in inflammatory skin conditions like acne and psoriasis. These fats are especially abundant in cold water fatty fish like sardines, salmon, mackerel, tuna, anchovies, and cod.
5. Take supplements
Adding the right high quality supplements to your diet will help ensure you don’t become deficient in the vital dietary elements that contribute to healthy skin. Consult with your physician to properly determine which supplements, if any, make the most sense for your specific situation.
- Vitamin C — The antioxidant properties of vitamin C, combined with its role in the production of collagen synthesis, make it essential for good skin health.
- Vitamin E — Vitamin E limits the damage free radicals inflict upon the body, thereby helping to keep skin supple and youthful.
- Vitamin A — Vitamin A encourages healthy skin cell production and stimulates fibroblasts in the dermis that are responsible for the development of skin tissue.
- B vitamins — B vitamins are thiamin, riboflavin, niacin, folate B6, B12, biotin, and pantothenic acid. They improve the ability of the uppermost layer of the epidermis to retain moisture – leading to softer, smoother skin with less dryness and flakiness. It also plays a crucial role in the cell reproduction of the skin, nails, and hair. Vitamin B12 in particular soothes the skin, reducing redness, dryness, inflammation and acne blemishes, and is a highly recommended nutrient for sufferers of psoriasis and eczema.
6. Don’t scratch
The temptation to scratch at dry, peeling skin caused by eczema can be insistent, but scratching leads to complications; opening small cracks and wounds that become vulnerable to bacteria and infections.
7. Use hypoallergenic skin products
Shampoo, makeup, perfume, and cologne can trigger anything from a rash to a full-blown allergic reaction. So consider using natural products that are more gentle on your skin. A general rule of thumb is that the fewer ingredients a product contains the better it is for your epidermis.
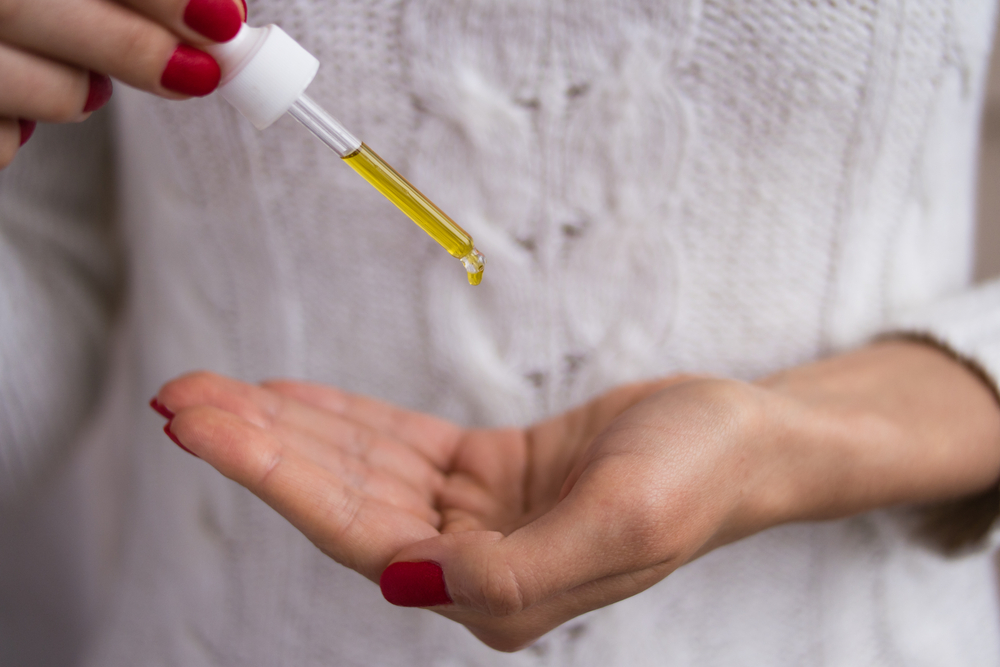
Can Essential Oils Replace Corticosteroids?
Anecdotal evidence suggests topically applied healing oils can reduce skin inflammation while increasing the skin’s moisture barrier. Holistically, essential oils are used to treat some of the underlying issues at play during eczema and psoriasis flare-ups. Among these essential oils are:
- Lavender
- Peppermint
- Eucalyptus
- Tea Tree
- Roman Chamomile
- Lemon
- Frankincense
- Sesame
In a recently published review of the therapeutic benefits of plant oils, the International Journal of Molecular Sciences states that these natural treatments are now being “increasingly recognized for their effects on both skin diseases and the restoration of cutaneous homeostasis.”
Among other benefits, the study concludes that many of these topical oils show anti-carcinogenic and anti-inflammatory potential. In some cases they may also promote wound healing and stop the growth of harmful microorganisms.
Conclusion
Patients who remain on low potency topical creams for chronic conditions need not be overly concerned with potential complications occurring. Negative side effects from corticosteroid are rare. However, this is conditional upon patients paying strict adherence to their physician’s directions on the correct use of topical steroid creams.